The overwhelming majority of the patients I’ve encountered on the wards have diabetes mellitus (DM). While there are countless ways to manage DM as an outpatient (insulin injections, biguanides, sulfonylureas, etc.), sliding scale insulin (SSI) seems to be the most routinely used method of controlling blood glucose (BG) for hospital inpatients. SSI provides patients with a dose of short-acting insulin based on their pre-meal glucose reading (typically four times a day).
Enter the RABBIT 2 Trial.1
In a randomized, multicenter, prospective study of 130 patients split evenly into two cohorts of 65 individuals from the general medicine ward population, researchers attempted to assess the efficacy of SSI to a “basal-bolus” insulin regimen. As far as the demographics go, these patients ranged from 18 to 80 years of age and were previously treating their diabetes with either oral hypoglycemic drugs or solely dietary modifications. In other words, this is the first time the patients would be given insulin injections to control their DM. No patient follow-up information was included in the study.
BASAL-BOLUS REGIMEN
Daily insulin requirement based on admission BG: 0.4 units/kg for BG 140-200 mg/dL and 0.5 units/kg for 201 mg – 400 mg/dL
Half the required insulin would be glargine (a very long-acting insulin) given at the same time every day. The other half would be divided into 3 equal doses of glulisine (short-acting insulin) and given once before each of three meals. The glulisine was held if the patient could not eat. The glargine dose was increased or decreased by 20% if the premeal blood glucose was >150 mg/dL or after an episode of hypoglycemia (<70 mg/dL), respectively.
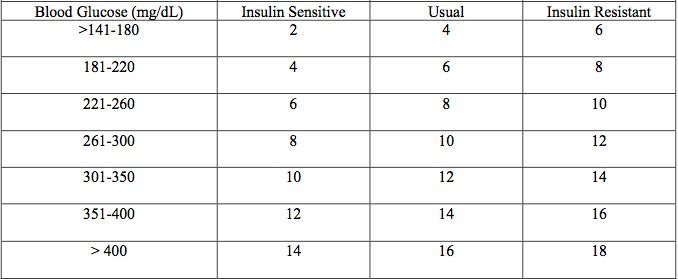
SLIDING SCALE PROTOCOL
Patients received regular insulin four times a day for BG > 140 mg/dL. If patient couldn’t eat, insulin was given every six hours to avoid hypoglycemic event. If pre-meal BG >140 mg/dL, requirements were shifted to “Usual” or “Insulin Resistant” values. If the average BG was >240 mg/dL, patients were actually transitioned to the Basal-Bolus protocol and started on 0.5 units/kg. Seems like the researchers already knew which protocol was better going into the trial. 😉
HbA1c was measured on admission and BGs were measured before each meal (every 6 hours if NPO). The whole point of the study was to keep patients below a BG of 140 mg/dL. The following table summarizes the important findings of the RABBIT 2 trial:
| Basal/Bolus | SSI | |
| Admission BG | 229 ± 71 | 225 ± 60 |
| Avg. BG during stay | 166 ± 32 | 193 ± 54 |
| Avg. fasting BG | 147 ± 36 | 165 ± 41 |
| Avg. random BG | 164 ± 35 | 188 ± 45 |
Given the two cohorts of DM patients with similar admission BGs, the basal-bolus regimen provided statistically significant improvement of hyperglycemic control (<140 mg/dL) over the SSI group.
1. “Randomized Study of Basal Bolus Insulin Therapy in the Inpatient Management of Patients with Type 2 Diabetes (RABBIT 2 Trial)” – http://care.diabetesjournals.org/content/early/2007/05/18/dc07-0295






As a Registered Dietitian and Certified Diabetes Educator working in an endocrinology practice for over 15 years, I can say that patients can and do learn how to Carb Count. It improves BG control, and gives the patient confidence in taking control of their BG. In a LTC setting (Cayuga Ridge Healh & Residential Community, Ithaca, NY) beginning over one year ago, nursing began using BBC regimen with great success and ease. A controlled amount of carbs are provided with meals allowing pc rapid-acting insulin analogue based on % meal intake eg., 4 units at 100% po, 3 u 75%, 2 u 50% po etc., and added to this an Insulin Correction dose written in the form of sliding scale, but determined with the 1800 Rule. In a hospital setting there may be meal tickets with pre-printed CHO g making this process even more effective by dosing based on a more precise insulin:CHO ratio.
Basal/Bolus sounds like it would be great in the hospital, if the nurses don’t get annoyed with you for ordering it. Not sure about sending the patient home with those instructions. They would definitely be less compliant. In the end, order what is best for the patients.
Thank you for the informative, timely article! I was just wondering about DM pts that are seen in hospitals from a conversation I had with a doctor while volunteering last week.