The indications for central venous catheters (CVCs) include invasive hemodynamic monitoring, transvenous cardiac pacing, hemodialysis, lack of peripheral venous access, administration of vasopressors, nutritional support, and in some texts…. volume resuscitation. It’s this last one that bothers me. Yes, some CVCs like multi-lumen access catheters (MAC) can be wonderful for massive resuscitation, but the traditional CVC is horrible compared to large bore peripheral intravenous (PIV) catheters. Let’s look at this in terms of catheter flow rates.
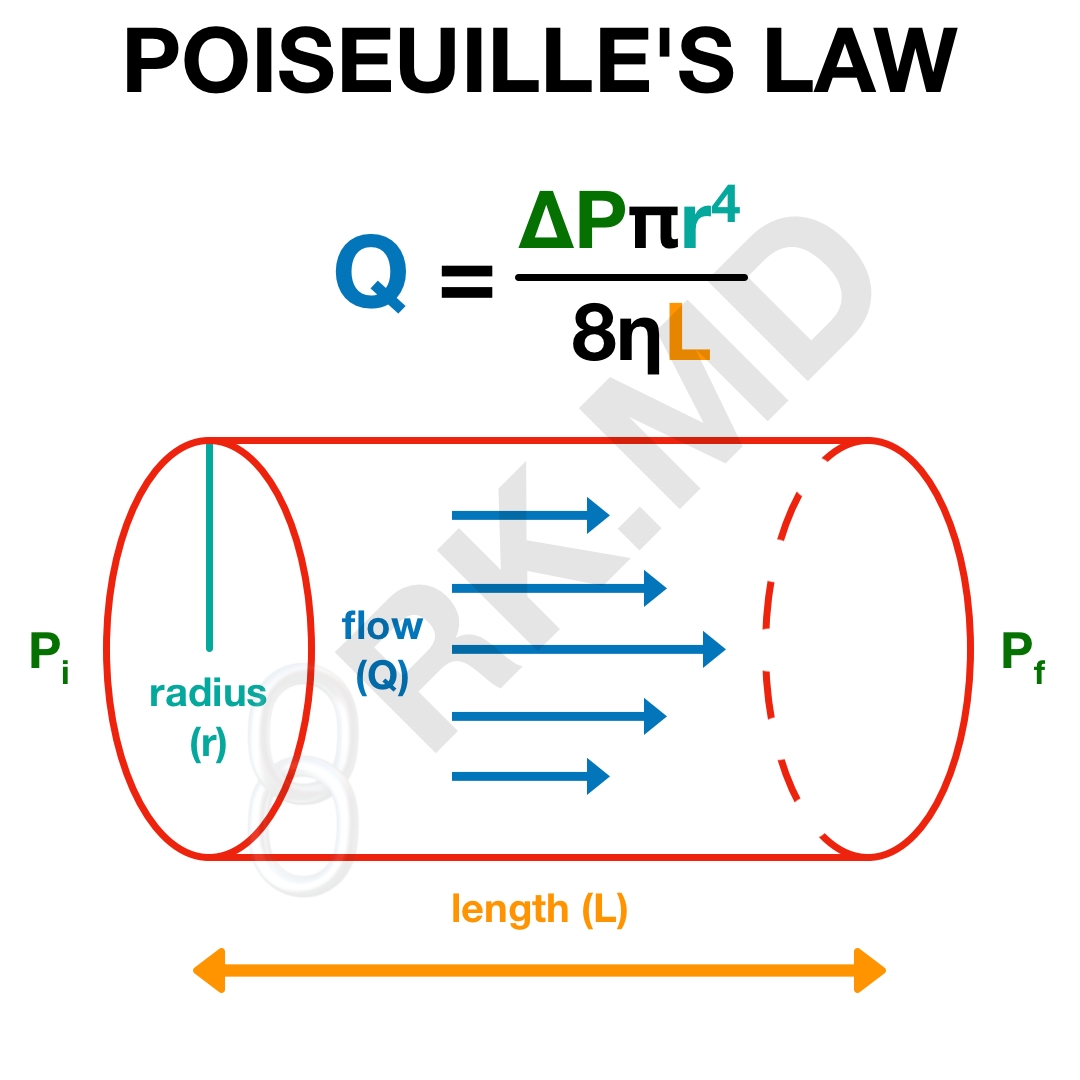
Poiseuille’s Law describes the dynamics of laminar fluid movement through a pipe much longer than its diameter and is given below.
In essence, as our catheter’s length increases (think of 20 cm CVCs compared to ~ 3 cm PIVs), flow will be reduced. More importantly, as the catheter’s radius increases (lower gauge sizes, higher French sizes), the flow rate increases by a power of 4. Clearly, this is the most important factor in determining overall flow.
Pictured, you see 16G, 18G, 20G, and 22G Terumo PIV catheters with flow rates of 198 cc/min, 100 cc/min, 60 cc/min, and 35 cc/min, respectively. In comparison (and depending on what you read), a central line which includes a 16G lumen has a rate of approximately 70 cc/min. This is substantially different from the almost 200 cc/min we get with a 16G PIV.
Manufacturers often list flow rates through their catheters, but in general, I’ve found large bore PIVs to be superior to most central lines for volume administration. I’ll never forget a case where I placed two 14 gauge PIVs for a patient with known placenta accreta, a case where copious bleeding is anticipated. Those lines ran like fire hoses! 🙂
Next time you place a central line for “volume resuscitation”, look at the actual packaging and consider how the length of the catheter, lumens, and even IV tubing (extensions, stopcocks, adapters) will affect your overall flow rate. We’re usually better off avoiding the risks of CVCs (pneumothorax, arterial injury, air embolism, catheter-related bloodstream infections, etc.) and placing large bore PIVs instead. 🙂








Does the long and small peripheral vessel count for the equation, because CVC is better in that it reach large vessel. I think that the best is short large bore at jugular.
The fluid still has to go through the catheter first, so having a long central line in a large vessel won’t be as good as a short, large bore catheter in a large vessel.
Do you have any way to measure peripheral vascular resistance?
Using pressure infuse bags will increase the flow even more and cvcs can be used for volume resuscitation of they are there only access possi of
This is true, but pressure infusion bags will also increase flow even more across a catheter that’s better suited for high flow rates (large, short catheters like 14 gauge peripheral IVs).
Totally agree , because of poiseullie’s law presure is the last option to increase bat can be appled to both central and peripheral catethers
Well well, can’t differ in this point… I remember being in charge of a child undergoing a tibial osteosarcoma removal, a surgery with a lot of bleeding as well, I took a 20 G in the forearm and an 18 G external jugular…. Still got blamed by my attending for not taking a CVC, told him that I have readied the gear if needed. Problem with PIV is that you can’t give catecholamines through them, apart from dobutamine and epinephrine….
Speaking now of manufacturers, we use the ARROW. CVC in our workplace. I love the 7F models, the wire is of good quality but the smaller ones 4F for instance are quite tricky to use…. what do you use over there for small children?
Keep the hard work up
I actually don’t remember what size/brand of CVC we use for our pediatric patients (been a while since I’ve done a central line in a child), but we use a variety of lines in adults (some are pictured in the post). Haha, and you know we’ll get blamed from time-to-time… it’s the nature of residency. 😉