Point-of-care ultrasound (POCUS, “bedside ultrasound”) is useful for so many things in the intensive care and perioperative settings. I routinely utilize POCUS to assess my patients’ cardiac contractility, intravascular volume status, valvular pathologies, and the like. POCUS lets me see, real-time, how titrating certain pressors/inotropes, arrhythmias, and/or giving fluids directly affects cardiac output.
I always harp on the need to be extremely critical of what an image, lab value, or monitor reading suggests in the context of its limitations and pitfalls.
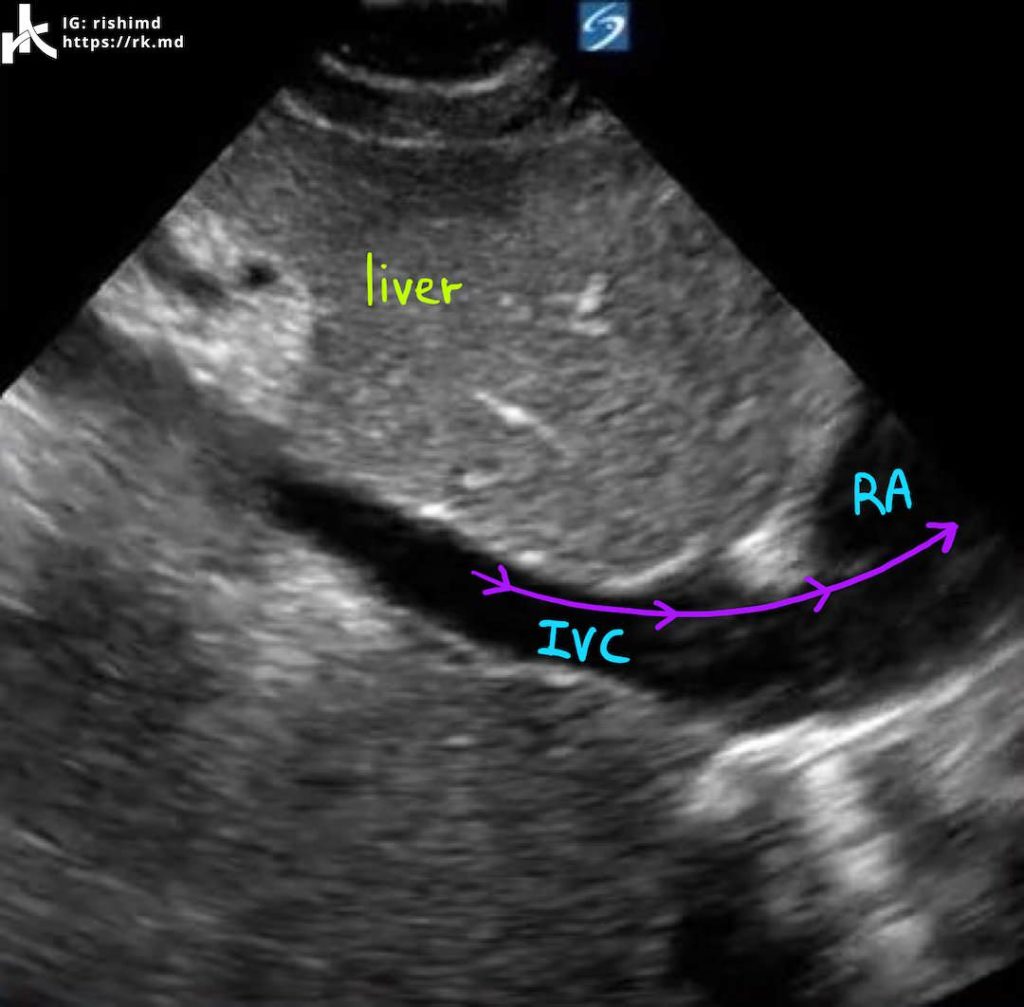
Above, you see a subcostal view of the inferior vena cava (IVC) in long axis showing very little variability in diameter with the respiratory cycle. This suggests intravascular volume adequacy; however, remember that the IVC drains into the right atrium (RA). If anything impedes forward flow into the RA or promotes backflow from the RA, the IVC might also appear full.
I proceeded to examine the heart itself. Here’s what an apical four chamber view should look like:
I acquired an apical view (4/5 chambers) with and without color. Remember the ultrasound transducer is at the top of the screen firing downwards. Flow moving towards the transducer appears red and flow away is blue. What do you see?
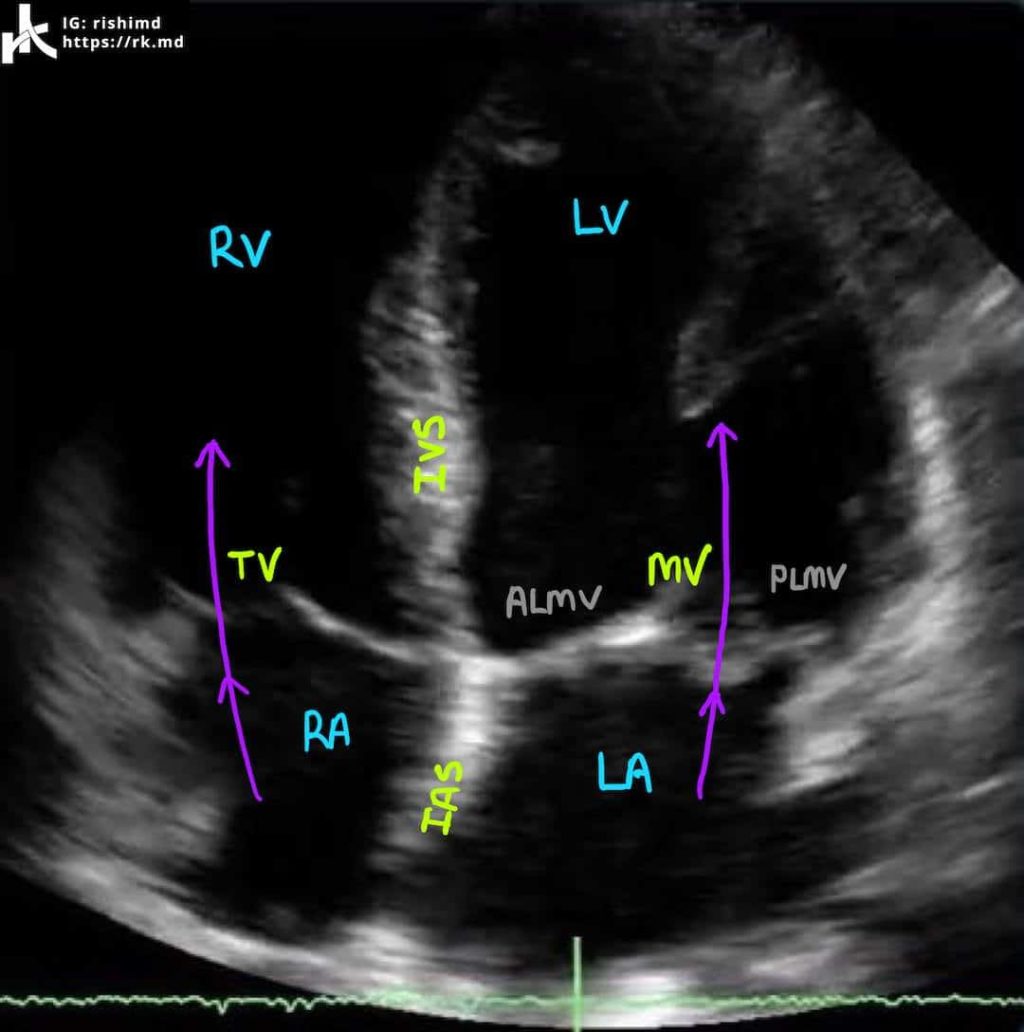
Without going into the measurements or other echo windows, you’re seeing severe tricuspid regurgitation and moderate-severe mitral regurgitation. With all that tricuspid regurgitant volume making its way from the right ventricle into the right atrium, there’s definitely a higher-than-normal right atrial pressure which can cause the IVC to appear full… regardless of the patient’s volume status. Also note how the enlarged RV is “apex forming!”
It’s important to keep this in mind when looking at the IVC on ultrasound. We can see similar findings with pulmonary hypertension, right heart failure, etc. Drop me a comment below with questions! 🙂





