In my first year of anesthesiology residency, I had the opportunity to do a very unique aortic valve replacement (AVR) case for aortic stenosis – the Ozaki repair performed by Dr. Ozaki himself! This incredible surgeon pioneered a technique using the patient’s own pericardium (lining that surrounds the heart) treated with glutaraldehyde to construct an autologous aortic valve which does not have the immunologic implications of foreign, prosthetic material nor the need for anticoagulation.
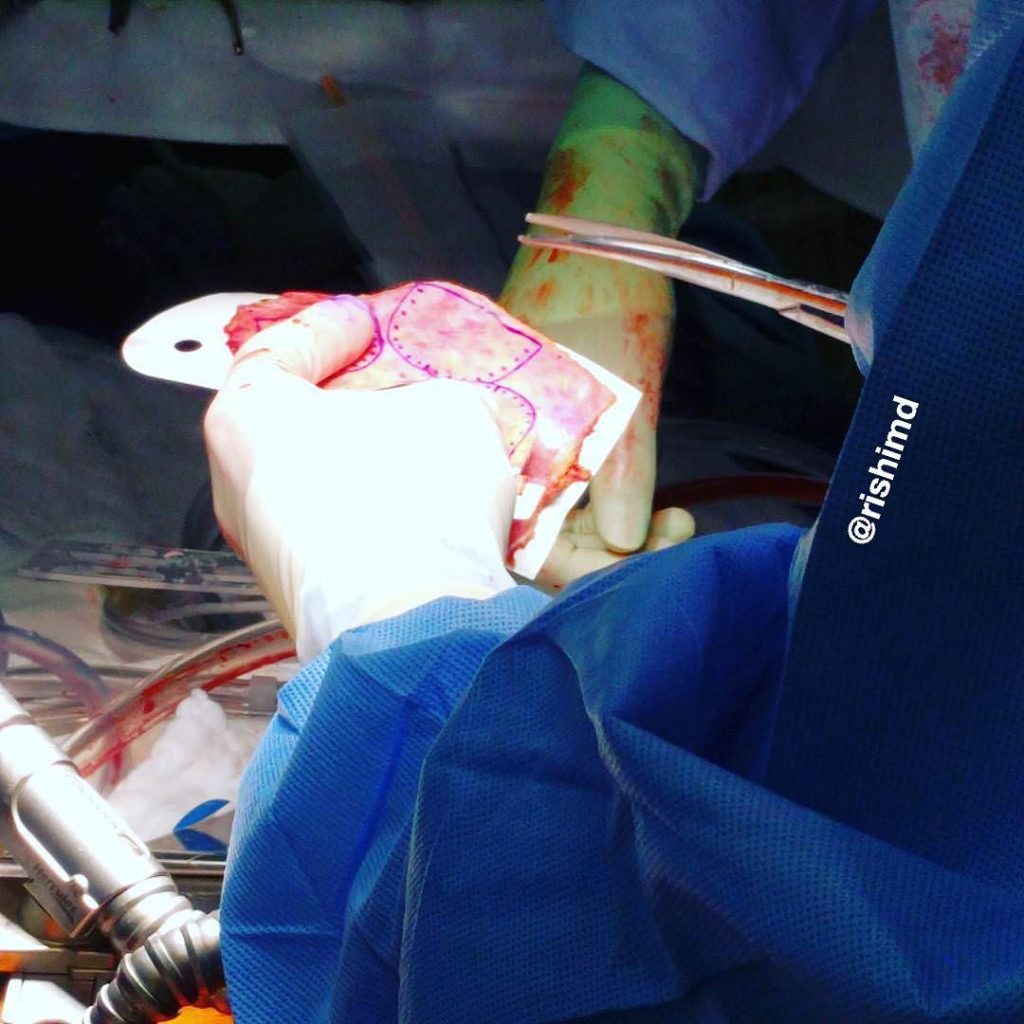
Pictured is the harvested pericardial patch with aortic valve cusps sized/traced onto it. These cusps are then trimmed and sewn into the native aortic annulus creating a characteristic “windmill” shape that facilitates valve coaptation.
At that point in my training, I was just hoping not to intubate the esophagus or blow my peripheral IVs; however, I was immediately captivated by cardiac surgeries, the complex pathophysiology/pharmacology of cardiothoracic medicine, intraoperative echocardiography, and the calm demeanor of my mentors. It was at that time I knew I wanted to do at least one fellowship – fast forward five years later, and now I’m living it… with a little more understanding! 🙂





