Medical trainees are taught how to listen to patients’ chief complaints and decide how to pursue a diagnostic work-up. Atypical chest pain, acute appendicitis, kidney stones, and a myriad of other diagnoses all have particular “classic symptoms” patients often reference in their history; however, what happens when patients can’t talk to you? When they can’t tell you exactly where it hurts or what they’re feeling? How do you catch acute changes which could potentially be life threatening? These are all challenges faced during general anesthesia.
As an anesthesia provider, I devote my full attention to the safety of my patients by troubleshooting change. What if their blood pressure drops? What if their heart rate increases? What is their body trying to tell me while anesthetized?
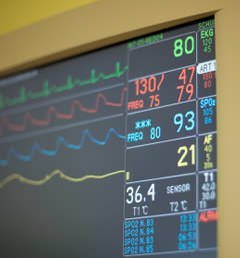 Let’s consider an example… acute onset tachycardia (fast heart rate). Did it coincide with a particularly stimulating or painful part of surgery? If so, maybe it’s due to pain. How about a concordant drop in blood pressure? Maybe you’re seeing a reflexive tachycardia and the patient needs more fluid resuscitation. Is the patient going into alcohol withdrawal? Did they develop a pulmonary embolus? Maybe they’re “light” under anesthesia and are trying to wake up? These possibilities are only a handful of things we consider for a simple bump in heart rate.
Let’s consider an example… acute onset tachycardia (fast heart rate). Did it coincide with a particularly stimulating or painful part of surgery? If so, maybe it’s due to pain. How about a concordant drop in blood pressure? Maybe you’re seeing a reflexive tachycardia and the patient needs more fluid resuscitation. Is the patient going into alcohol withdrawal? Did they develop a pulmonary embolus? Maybe they’re “light” under anesthesia and are trying to wake up? These possibilities are only a handful of things we consider for a simple bump in heart rate.
The wonderful thing about this profession is that we’re constantly making small adjustments and administering medications with immediate feedback. In the example above, if a patient’s heart rate jumped with Mayfield skull pin placement, I’d deepen the anesthetic with an opioid adjunct. In no time, I’d be able to tell if that made a difference. More importantly, next time, I’ll anticipate this reaction and prepare the patient ahead of time.
Astute anesthesiologists are skilled in rapidly diagnosing and properly treating flux in the unconscious patient. I hope in the coming months I’ll gather even more experience in recognizing subtle variations in my patients’ clinical status.





