The subcostal view on transthoracic echocardiography can be used to examine the inferior vena cava (IVC), a large valveless vein that returns blood from the lower body to the right atrium (RA).
With spontaneous inspirations, the diaphragm contacts downward generating a negative intrathoracic pressure and drawing blood from the superior vena cava (SVC) and IVC into the RA. This, in return, will partially collapse the IVC as it is emptied. In comparison, intubated patients on positive pressure ventilation will increase their intrathoracic pressure during inspiration and push blood out of the heart into the IVC. In either situation, the magnitude of IVC change during breathing roughly corresponds to intravascular volume status. In other words, a patient who is intravascularly overloaded will not have significant variability (collapse nor distension) during breathing.
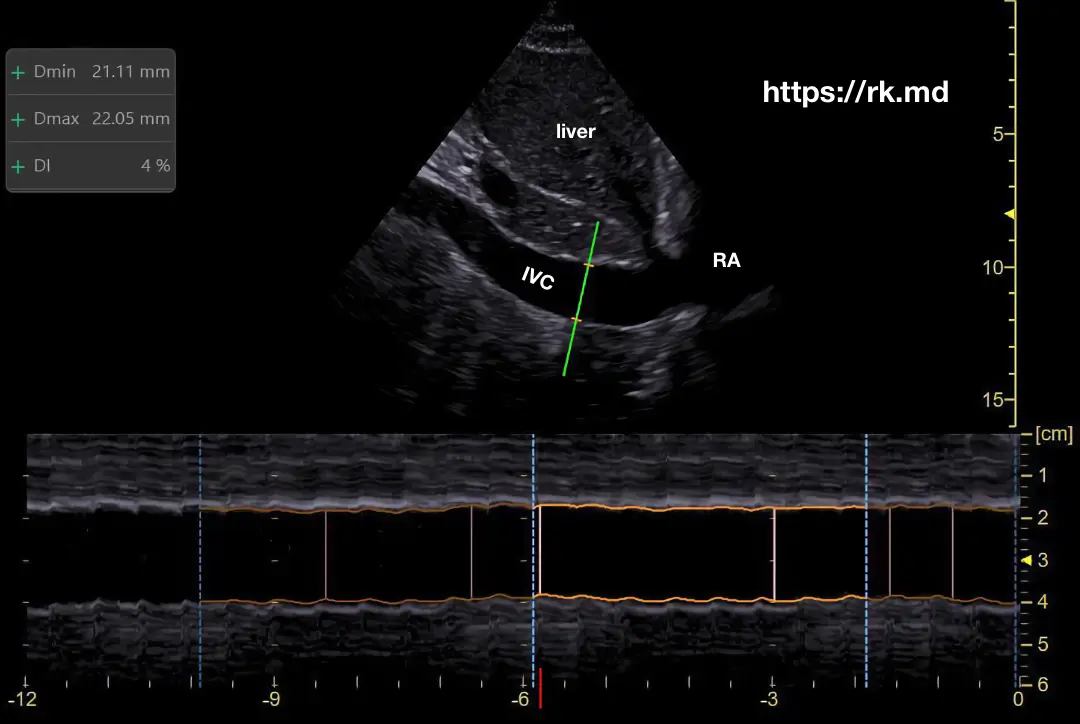
Remember that anything that increases right atrial pressure can be back transmitted into the IVC (ie, pulmonary hypertension, tricuspid regurgitation, thrombus, etc.) Additionally, the ultrasonographer’s experience and skill level affects the quality of IVC measurements.





