I’ll be spending the next two months at Texas Heart Institute, a nationally-recognized institution pioneering and delivering unparalleled care in cardiothoracic medicine and surgery. So far I’ve done a home call, in-house call, and a “regular day” before having another in-house call shift tomorrow. The cases here are incredible, and the attendings are much more focused on the overall picture rather than nitpicking about small details – I guess it’s a perk with being a more senior resident. 🙂
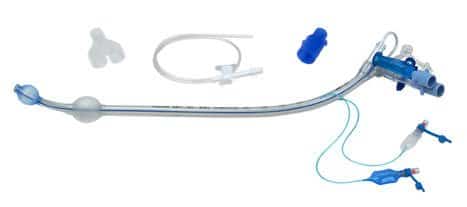
Certain surgeries (thoracic aortic aneurysms, lung resections, etc.) require anesthesiologists to ventilate each lung independently using a double-lumen endotracheal tube (DLT) or bronchial blocker, and for periods of time, collapse one lung entirely for the surgeons to operate. This is known as one lung ventilation (OLV) and has a myriad of pharmacologic and physiologic implications.
It makes sense that one’s ability to oxygenate and ventilate are compromised when only one lung is being used. The body does a great job of compensating by preferentially shunting blood flow to the ventilated lung (known as hypoxic pulmonary vasoconstriction), but sometimes patients began to desaturate depending on the nature of the surgery, preexisting lung pathology, positioning, etc. The typical textbook options to improve hypoxemia during OLV include:
- Applying positive end-expiratory pressure (PEEP) to the dependent (nonsurgical, ventilated) lung
- Applying continuous positive airway pressure (CPAP) to the nondependent (surgical, unventilated) lung
- Going back to two lung ventilation
- In dire situations, clamping the pulmonary artery supplying the surgical lung
Applying CPAP to the surgical lung will definitely help with oxygenation but at the expense of compromising surgical exposure and often times safety. In other words, it’s hard to resect a lung when it keeps expanding and contracting with each breath.
Another option which I’ve learned is placing a catheter several centimeters down the DLT connected to low-flow oxygen. This will provide passive oxygenation down a pressure gradient into the unventilated lung. The oxygen flows are so low (1-2 liters/min) that the lung shouldn’t expand all that much, so the surgeons can work uninterrupted. It’s not CPAP, per se, but you still get more alveoli to work with by sending oxygen down the unventilated lung. 🙂





