Asleep-awake-asleep craniotomies aim to preserve portions of the eloquent cortex – parts of the brain that are critical for speech, language, motor function, and localization. Patients are awake for brain surgery. I wanted to give a play-by-play of the anesthetic considerations.
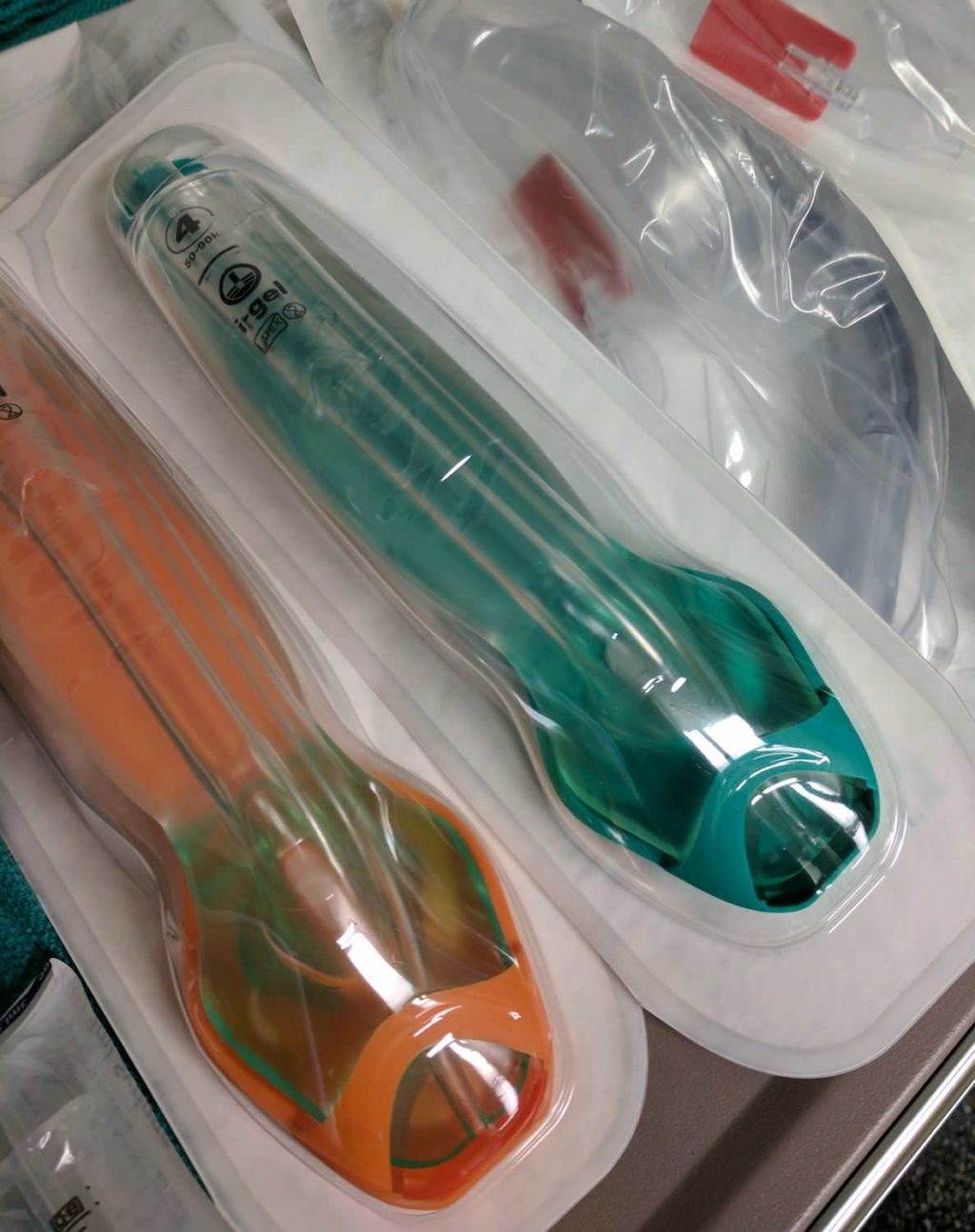
First, the patient entered the operating room and was positioned in their final surgical position with a bump under one side of the head to elevate the operative side. After preoxygenation in this awkward position, I performed a standard intravenous induction of general anesthesia with 1 mg/kg of lidocaine, 1 mcg/kg of fentanyl, and 2 mg/kg of propofol. I placed a laryngeal mask airway (LMA) and started the following infusions for my total intravenous anesthetic (TIVA):
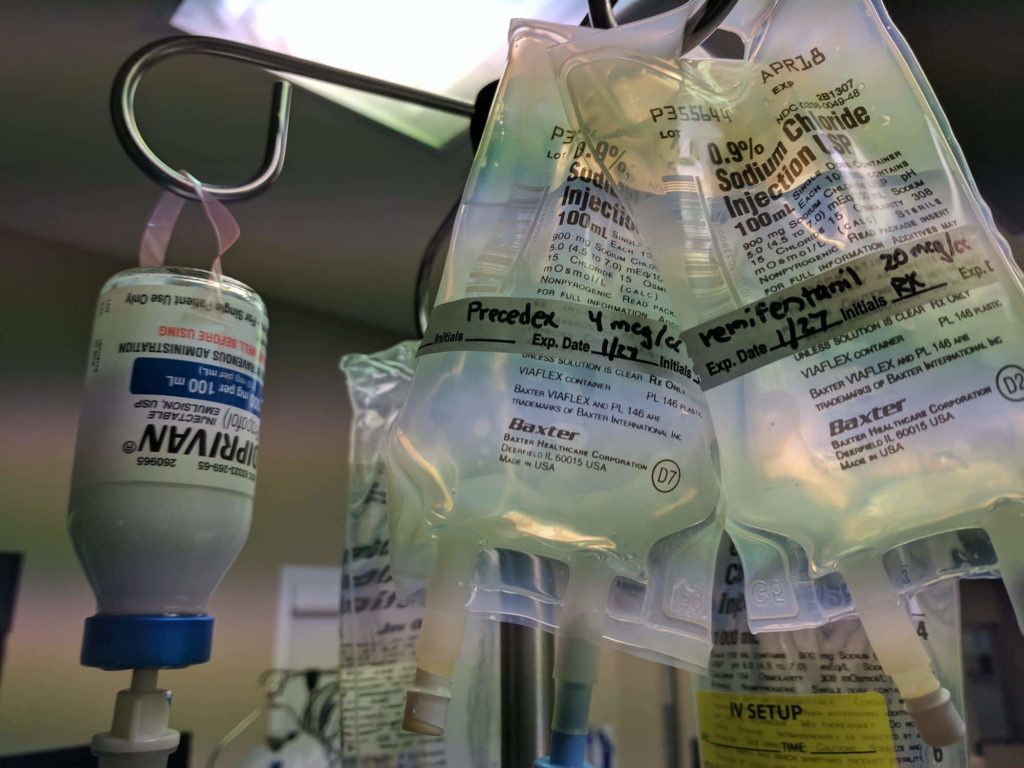
- dexmedetomidine: 0.5 mcg/kg/hour
- remifentanil: 0.2 mcg/kg/min
- propofol: 75 mcg/kg/min
I then placed a second peripheral IV and arterial line just before the surgeons performed a scalp block and placed the Mayfield skull fixation device, an intense stimulus which I offset with 1 mg/kg of propofol and 1 mg/kg of esmolol. At this point, the patient was asleep, maintained on infusions, and the surgeons began their craniotomy.
Once the dura was accessed and brain surface was exposed, I began to lighten the depth of anesthesia by turning off the propofol and remifentanil drips and reducing dexmedetomidine to 0.2 mcg/kg/hour. In less than 10 minutes, the patient was breathing well and awake. I removed the LMA and suctioned the oropharynx in preparation for speech mapping.
As the neurosurgeons applied an electrical current to various portions of the exposed brain (remember, the brain itself has no pain receptors), a neurologist and neurophysiologist had the patient perform tasks like counting numbers and naming objects. If the electrical stimulus impeded on the task, that portion of the brain was flagged and preserved during dissection. This technique was used in conjunction with peripheral nerve monitoring. With a low dose dexmedetomidine infusion, patients are comfortable, conversing, breathing well, and have a stable hemodynamic profile.
After the speech mapping was completed and surgeons completed their tumor resection, I re-induced general anesthesia (standard propofol induction), replaced the LMA, and restarted all my infusions as above while the surgeons began closure. I stopped all my infusions just prior to scalp closure and removed the LMA immediately after the Mayfield pins were disassembled. Titrated in a little labetalol to keep the blood pressure appropriate, and bam… to the neuro intensive care unit we went!
Obviously, this procedure requires that patients remain calm in very tight and uncomfortable positions. Their heads are pinned. They’re still drowsy from the initial anesthesia. Their arms and legs might cramp. Their mouths might be dry. All things considered, a careful neuropsychiatric evaluation is conducted before attempting an awake craniotomy. This is where patient selection probably makes a HUGE difference! Oh, and a lot of verbal anesthesia during the “awake” phase.
I’ll never forget talking to my fully awake patient while over the drapes I see the surgeons resecting a brain tumor. Incredible! 🙂






Loved every word of this article and plan on keeping it as how-to recipe when facing a similar situation myself in the near future. I have sone questions nonetheless:
1- Why lido as part of the induction?
2- Is it part of your job to take care of the patient in th ICU?
3- How long did the procedure take? And why hasn’t the patient been intubated?
4-In the absence of dexmedetomidine which we are still to have in my country, can’t I us volatiles such as sevo?
Thanks for your insight pal and hoping to see more of these posts, though I don’t think they should be labeled pre-op screen. Pushing for a new categorie here…
1.) So in my training, we use lidocaine to sort of “blunt” the burning sensation of drugs like propofol and etomidate if they’re given through small, peripheral veins. I’ll hold pressure above the vein so the lidocaine can remain confined to the area of injection (sort of like a makeshift Bier block). Additionally, people cite that lidocaine helps blunt the sympathetic response to direct laryngoscopy too. Not really sure what the evidence is on this.
2.) We have dedicated neuro ICU teams that manage these patients post-operatively.
3.) Overall, the procedure took roughly 4 hours (about one hour of “awake” time). We typically don’t intubate these patients because performing laryngoscopy in pins and in the decubitus position can be fairly difficult. Plus I find that people just wake up cleaner with LMAs (ie, less coughing).
4.) Volatile agents can interfere with the neuromonitoring we perform on these patients. Plus, the “wake ups” aren’t as clean. Before dexmedetomidine, people used propofol infusions which worked fine but left patients a little foggy during emergence. It’s important that these patients wake up clearly, so they can participate in the neuro exam.
Thanks as always! I was thinking of just dropping the “pre-op screen” label and leaving the titles as they are.