The Frank-Starling law of the heart is one of the most important intrinsic properties of cardiac muscle. It states that a change in venous return (preload) confers a change in the force of cardiac contraction (stroke volume or cardiac output) through increased sarcomere lengthening and excitation-contraction coupling of the muscle fibers.
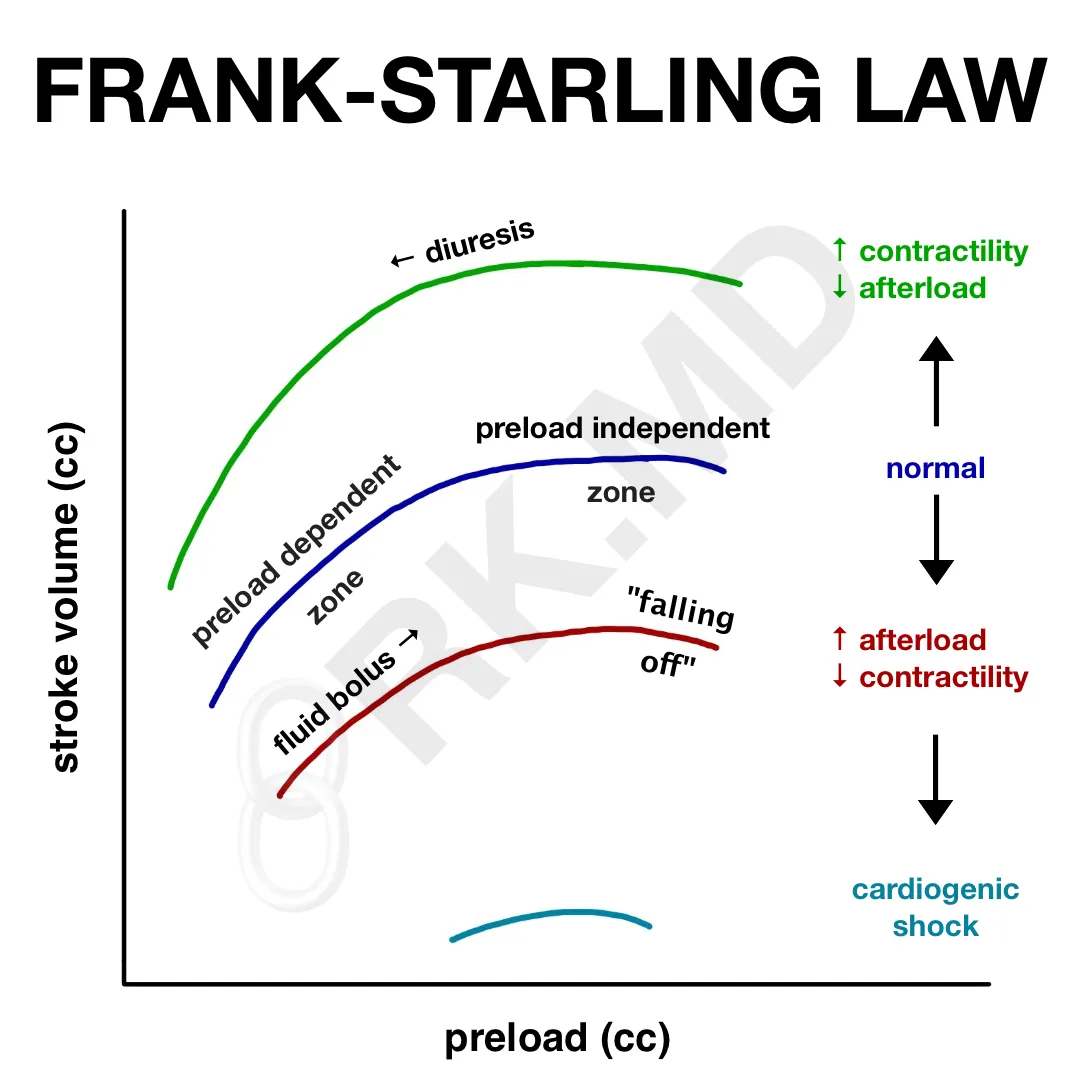
The ventricle operates on multiple Frank-Starling curves depending on the current afterload and inotropy. As these parameters are changed, the curves shift (see image). If afterload drops and/or contractility increases, the curve is shifted up and left. If afterload increases and/or contractility drops, the curve is shifted down and right. Along each of these curves, it’s possible to hold afterload and contractility constant while adjusting the preload through fluid boluses (rightward movement along a curve) or diuresis (leftward movement along a curve).
When we say patients are “falling off the Starling curve”, perhaps their ventricles simply cannot mobilize excess fluid. This results in a congested heart and decreased stroke volume. Maybe shifting leftward along the curve with diuresis would optimize our location on the curve back to a higher stroke volume? Or increase contractility and shift to a new curve entirely? This is where echocardiography comes in very handy! It’s easy to assess cardiac contractility, volume status, diastology, and filling pressures from this modality! 🙂
At the end of the day, we have no idea where our patients actually are on their respective Frank-Starling curves. We have to use the entire clinical picture to best ascertain which treatments should be attempted (inotropes, fluids, diuresis, afterload reduction, rate/rhythm control, etc.) based on their comorbidities, reasonable etiologies for decreased cardiac output, and response to therapy thus far.






Hi Could I get the picture of Frank Starling curve for free to my webpage of anesthesia and intensive care?
Best regards Kai Knudsen
Ph D, MD
Sahlgrenska University Hospital
Sweden
You can just download it from the post, but if you’re going to use my material, please leave the appropriate credit (link and watermark).
Hi, do you have a post where you’re talking about tidal volume? The combination of hypertension and hypercapni during general surgery? If not, can you please talk about it, maybe with one or three cases. Sorry my broke English. Thank you.
I’ll definitely keep this in mind! Stay tuned! 🙂