Patients with chronic thromboembolic pulmonary hypertension (CTEPH) present challenges from a surgical and anesthetic standpoint. They often have significant pulmonary collateral vessels to bypass obstructed pulmonary vessels. This, in turn, can increase bronchial vessel flow which can congest the pulmonary vessels even during bicaval venous cannulation. Additionally, large thromboembolic loads create large areas of dead space leading to V/Q mismatch with potential issues like hypoxemia and hypercarbia. This, in turn, can stress the right side of the heart leading to right ventricular pressure/volume overload, functional tricuspid regurgitation, elevated venous pressures, etc.
Pulmonary thromboendarterectomy (PTE) is the “gold standard” treatment for these patients. My anesthetic plan for PTE includes: general endotracheal anesthesia, arterial line (sometimes bilateral radial lines if anterograde cerebral perfusion is planned), central venous catheter with a PA catheter, inhaled pulmonary vasodilators (Veletri/Flolan) and intraoperative transesophageal echocardiography (TEE). In particular with TEE, I’m looking for signs of right ventricular failure, clots, an underfilled left ventricle, etc.
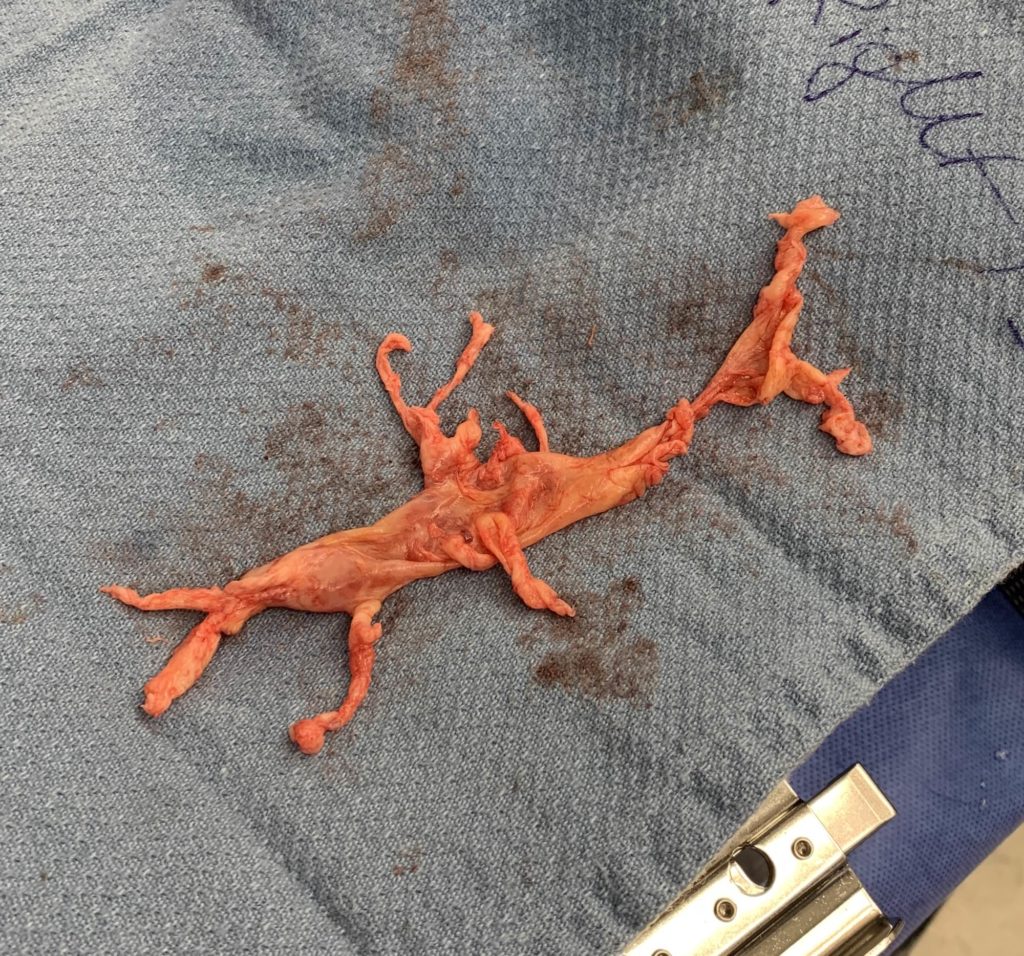
After a median sternotomy and systemic heparinization, the ascending aorta (arterial) and the SVC/IVC (bicaval venous) are cannulated in preparation for cardiopulmonary bypass (CPB). An aortic root vent is placed, and CPB is initiated. At this point, a left atrial vent is placed via the right superior pulmonary vein (RSPV), and cooling for deep hypothermic circulatory arrest (DHCA) is initiated. The right pulmonary artery (RPA) is opened with an endarterectomy carried to the segmental branches. A mirror procedure is performed on the left pulmonary artery (LPA).
Once we reach ~ 18-20°C, circulatory arrest begins and the remainder of the RPA endarterectomy is completed. Perfusion is resumed while closing the RPA. A mirror procedure is again carried on the LPA. DHCA allows the surgeon to have a bloodless field to optimize their endarterectomy. After rewarming, protamine administration, and CPB decannulation, hemostasis is achieved and the chest is closed in anatomic layers.
In the ICU, it’s important to watch for signs of reperfusion injury and remain judicious about volume administration.
Drop me a comment with questions! 🙂






When the cross-clamp comes off during CPB we usually administer either magnesium and/or lidocaine. During a PTE the cross-clamp might come off at 24C. Would you recommend waiting until the patient is somewhat warm to administer the cross clamp drugs or would you still give them while the patient is still cold?
I don’t think the timing has been studied, but my practice is to give it meds like lidocaine/magnesium closer to when weaning from CPB.
Hey Rishi.
Quick question for you. Regarding the coagulopathy that comes from DHCA in these patients who have poor RV function, do you often find is useful and/or necessary to utilize clotting factor concentrates like RIaSTAP or PCC in order to minimize the amount of volume given?
Thanks!
That’s a great question, Ben! As you can imagine, balancing coagulopathy with overly aggressive resuscitation in the context of a failing right ventricle is challenging. Visual inspection of the heart coupled with intraoperative echocardiography and invasive measurements (ie, PA pressures off a Swan) help determine how aggressive I can be. Often times I still find myself using FFP since many of these patients are overall volume depleted, but I’m more judicious about how fast I run it in. Additionally, I almost always have agents like epinephrine and inhaled pulmonary vasodilators to help mobilize the volume by optimizing RV function.