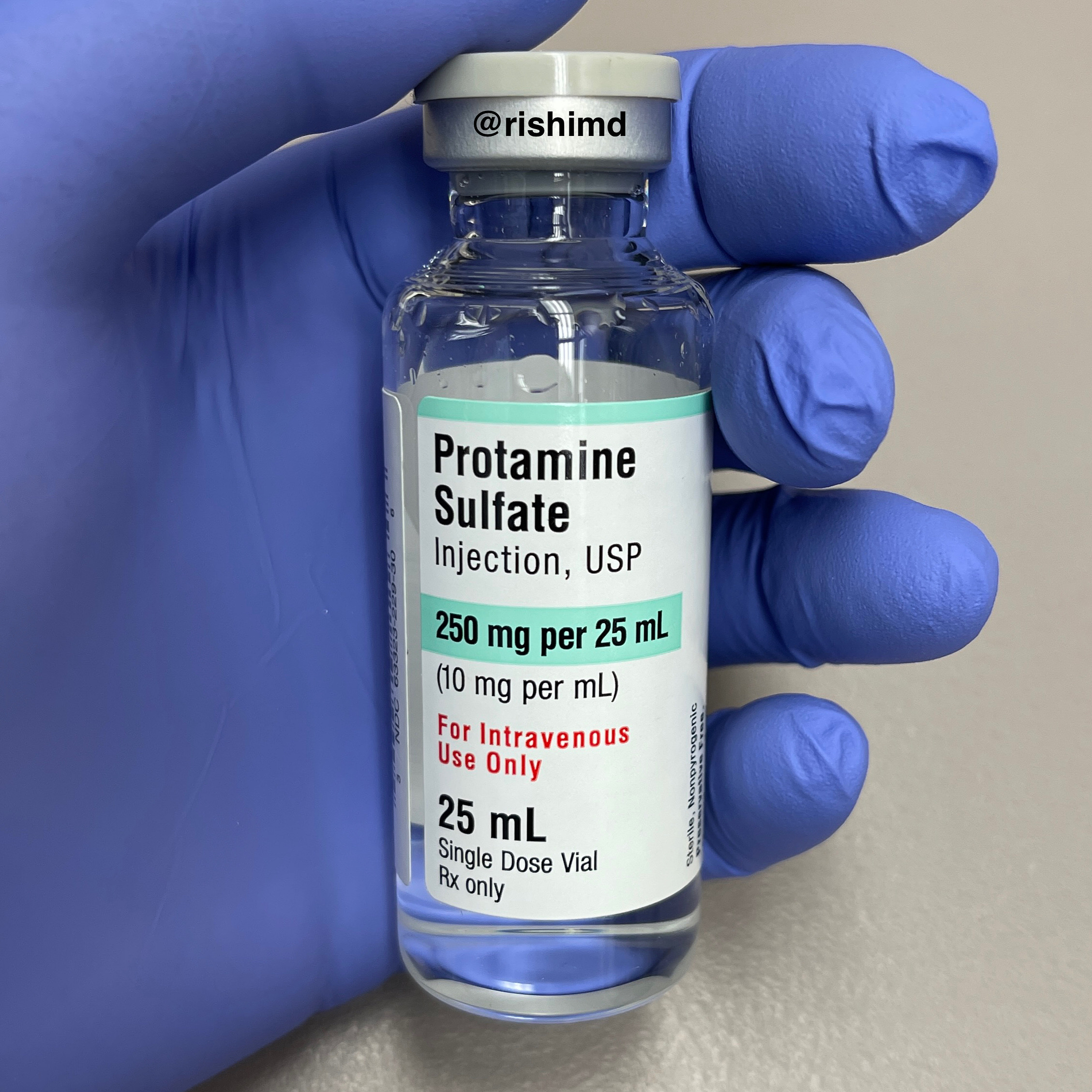
Protamine is an intravenous protein used to reverse the blood thinner heparin. This medication was initially derived from salmon sperm but is now synthesized with recombinant DNA technology. Heparin (negatively charged) forms an ionic bond with protamine (positively charged) creating inactive complexes metabolized by the reticuloendothelial system.
Protamine reactions are often classified as isolated hypotension (type I), anaphylactoid reactions (type II), and pulmonary vasoconstriction (type III). These are thought to be related to histamine release, nitric oxide generation, mast cell degranulation, complement activation, antibodies to protamine, and large heparin-protamine complexes. In addition, many references cite the following as risks for protamine reactions: fish allergies, taking NPH (neutral protamine Hagedorn) insulin, prior allergy to protamine, and vasectomy (due to the formation of anti-sperm antibodies, although the data doesn’t support this as a risk).
As a cardiothoracic anesthesiologist, I always administer protamine with a “test dose” when coming off cardiopulmonary bypass (CPB) to see how a patient’s hemodynamics change before slowly administering the total dose. Often, this requires supporting patients with volume, inotropes, and pressors. Rarely, severe pulmonary hypertension leading to cardiovascular collapse and acute RV failure may require reinitiating CPB. As a CVICU intensivist, I’ll also consider redosing protamine post-operatively (e.g., heparin rebound).
Drop me a comment with your experience regarding protamine!