Virchow’s triad of stasis, vascular damage, and hypercoagulability contribute to thrombosis. Although patients on extracorporeal membrane oxygenation (ECMO) are usually on pharmacologic anticoagulation (i.e., heparin), it’s still possible to form clots in areas of sluggish flow such as Y-connectors and the membrane oxygenator.
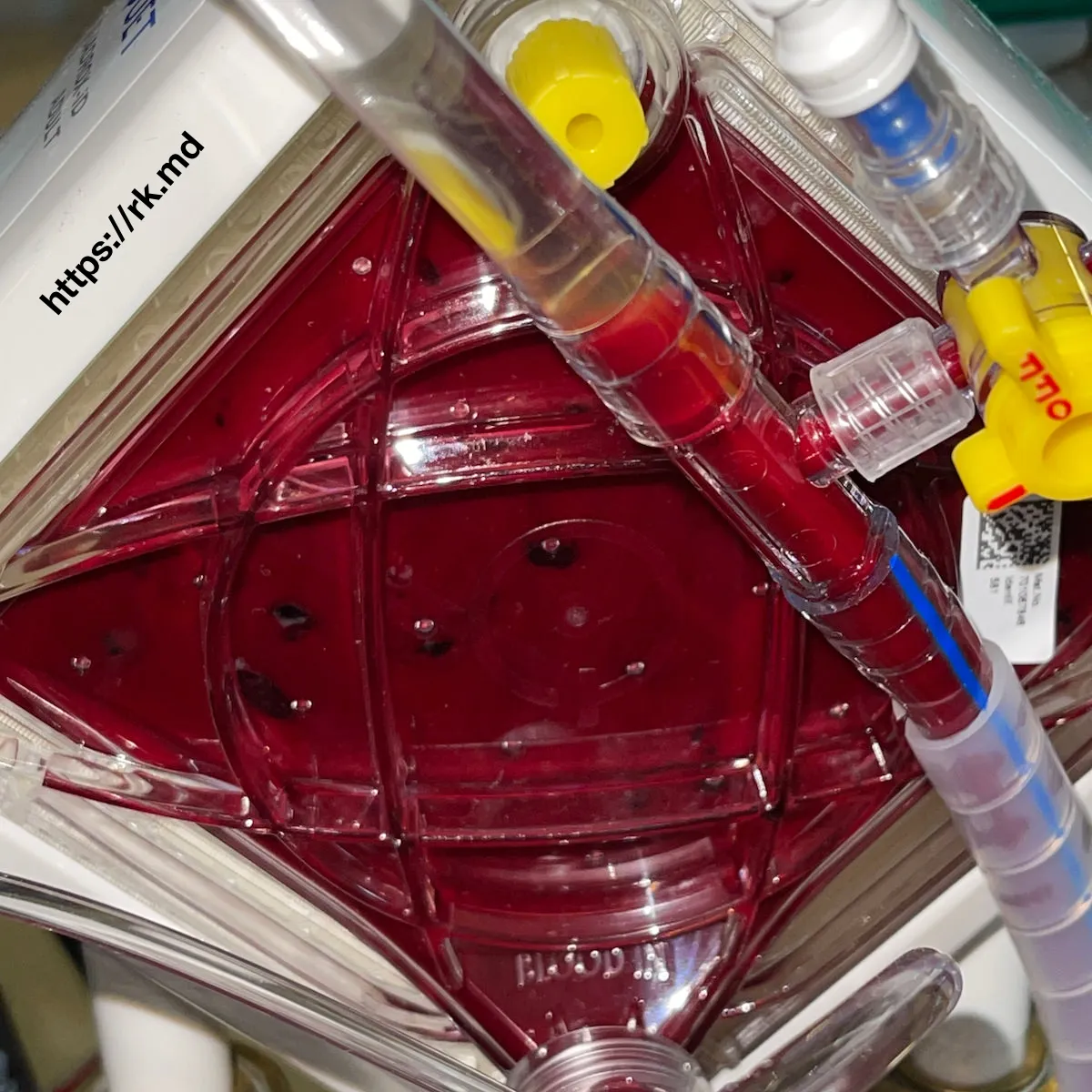
When I’m inspecting a circuit, I use a flashlight to assess for focal areas of clot formation which look like black spots as seen in the image. The upstream side of the oxygenator (specifically the corners) is usually where I find clots; however, one should carefully inspect both sides and the rest of the circuit. I’m especially concerned for clot formation in patients with hypercoagulable conditions such as a malignancy or situations in which the ECMO flow is low due to poor drainage, suboptimal cannula position, etc.
At a given pump speed, the pressure gradient across the oxygenator (ΔP) will start to increase as the clot burden worsens. Consequently, the ECMO flow may drop as more “work” is needed to overcome the increasing resistance. Conversely, if the pump speed is increased to improve flow, one runs the risk of increased hemolysis and “chattering” of the drainage line. Ultimately, the circuit may need to be changed.






Hello, I’m a perfusion new grad working in Texas. I cover ECMO at the hospitals here. In regards to clots present post-oxygenator, specifically the pigtail that is present at the top of the oxygenator, what should be done with clot formation? Should I refrain from flushing the pigtails, to avoid sending clots through the post-oxygenator? Is there another approach to fixing this problem? Possibly pulling the clot into a syringe instead of flushing forward?
Thanks for your help,
Alexander Diaz
Hey Alexander! That’s an excellent question, but one that I think would be better answered by one of your perfusionist colleagues, as I’m not actually sure what the best sequence of events would be in this situation. Please let me know what they say, as I’m also curious!