Targeted temperature management (TTM) following out-of-hospital cardiac arrest (OHCA) has been shown to confer survival and neuroprotective benefits. A 2016 review in Resuscitation found this to also apply to a wide scope of patients (unwitnessed arrest, persistent shock, non-shockable rhythms, etc.). Based on a 2013 NEJM RCT by Nielsen et al., there was no statistically significant difference in all-cause mortality in 950 unconscious patients presenting after OHCA with a TTM goal of 33°C versus 36°C.
In general, TTM is recommended for all patients with return of spontaneous circulation (ROSC) from cardiac arrest with altered consciousness post-arrest. The key is not to let these patients become febrile as there is an increase in neurologic demise.
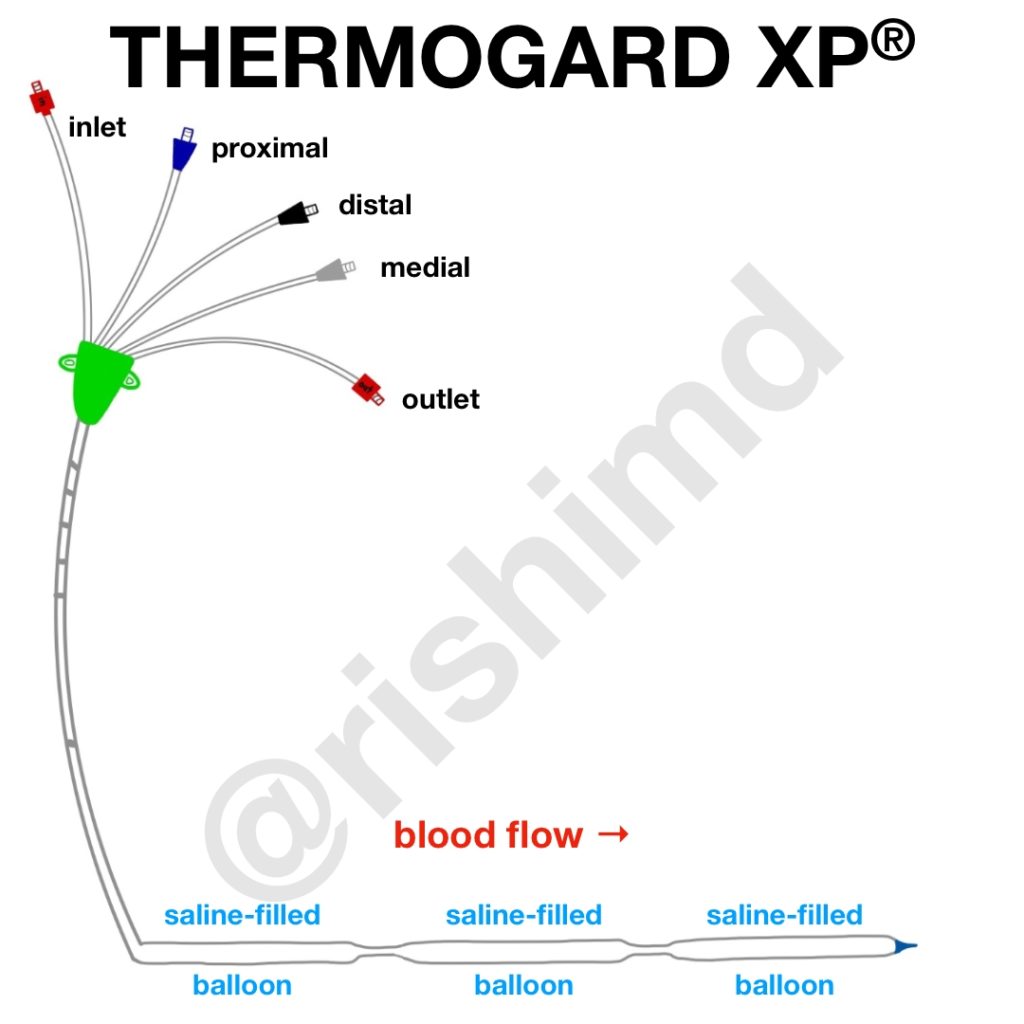
One technique for TTM is ZOLL’s Thermogard XP® catheter. This device combines a traditional triple lumen central line with a system of balloons filled with closed-loop, temperature-regulated saline via inlet/outlet tubing. This catheter is attached to a console which allows clinicians to quickly and precisely control a patient’s core body temperature. Typical TTM starts with early induction of cooling (ASAP), followed by maintenance for ~24 hours (varies based on the institution), and then slow rewarming (again, watch out for fevers!)
Cooling the core temperature of a patient necessitates sedation and sometimes even neuromuscular relaxation due to shivering. Furthermore, hemodynamic derangements (bradycardia, arrhythmias, decreased cardiac output/demand), altered drug metabolism (enzymes don’t do well in the cold!), and changes in electrolytes (hypokalemia is common) are commonplace.
Have you seen TTM utilized? How does your institution do it? Drop me a comment with your thoughts and questions!