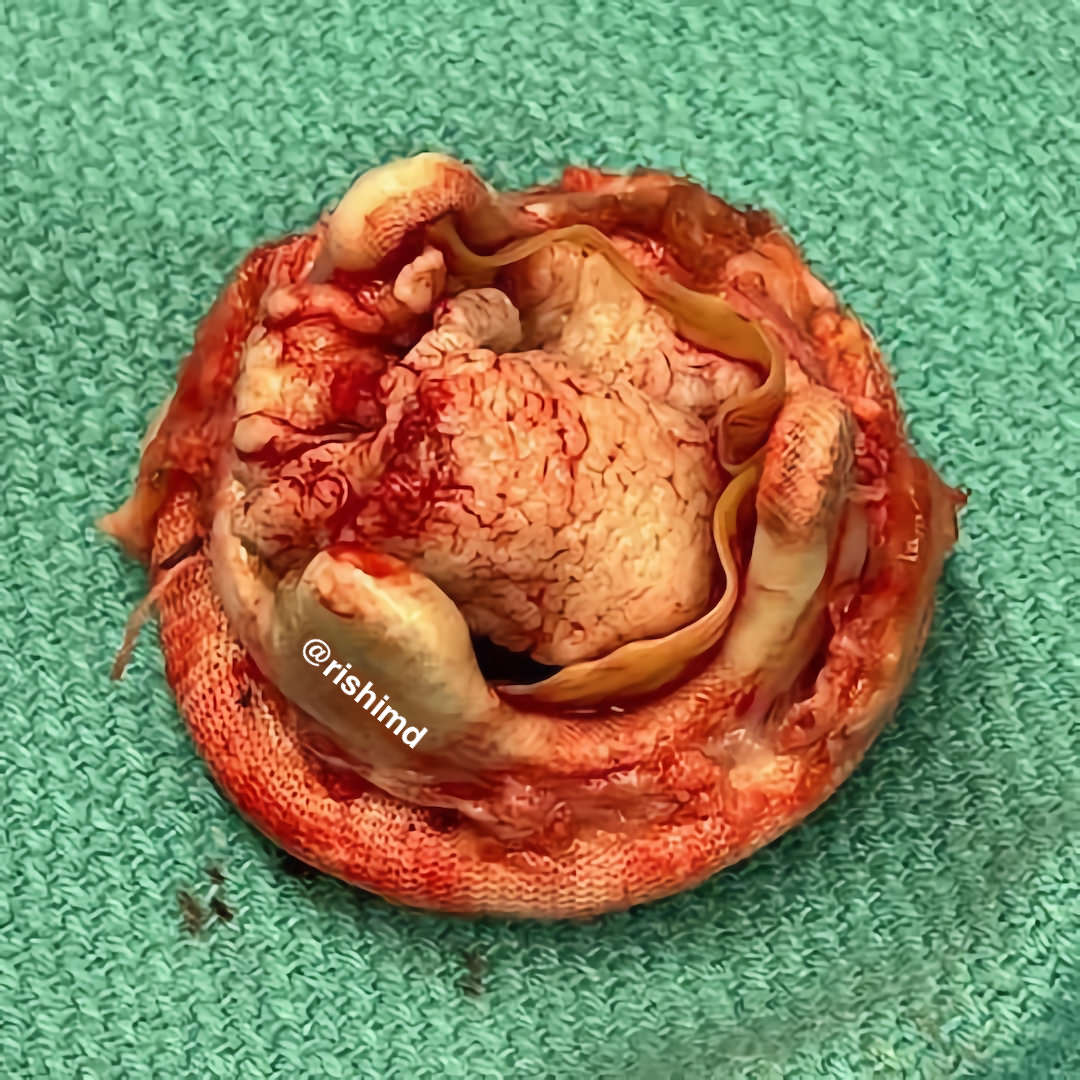
Fungal endocarditis (inflammation of the heart’s inner lining) is most commonly caused by Candida species and is associated with a high mortality rate. Risk factors include long-term antibiotic therapy (especially with indwelling central lines), immunosuppression, prosthetic heart material (valves, implantable devices, etc.), and IV drug use.
Like bacterial endocarditis, patients can present with a new murmur, fever, signs of congestive heart failure, peripheral embolic phenomena, and fatigue. This is an especially important diagnosis to recognize in patients with active candidemia as it can progress to endocarditis. Remember, yeast in a blood culture should NOT be considered a contaminant! Treatment includes early valve replacement and long-term antifungal medical therapy.
As an intensivist, I work with my infectious disease colleagues to initiate long-term antifungal therapies (usually a daily echinocandin like micafungin). As a cardiac anesthesiologist, I use transesophageal echocardiography to identify regions in the heart where damage has occurred, resulting in valvular regurgitation or abscess formation. In this video, one can appreciate a large vegetation on a bioprosthetic mitral valve that occludes the valve intermittently. In contrast to bacterial vegetations, fungal vegetations tend to be larger with more potential for embolization.
Drop me a comment with your experience regarding fungal endocarditis!