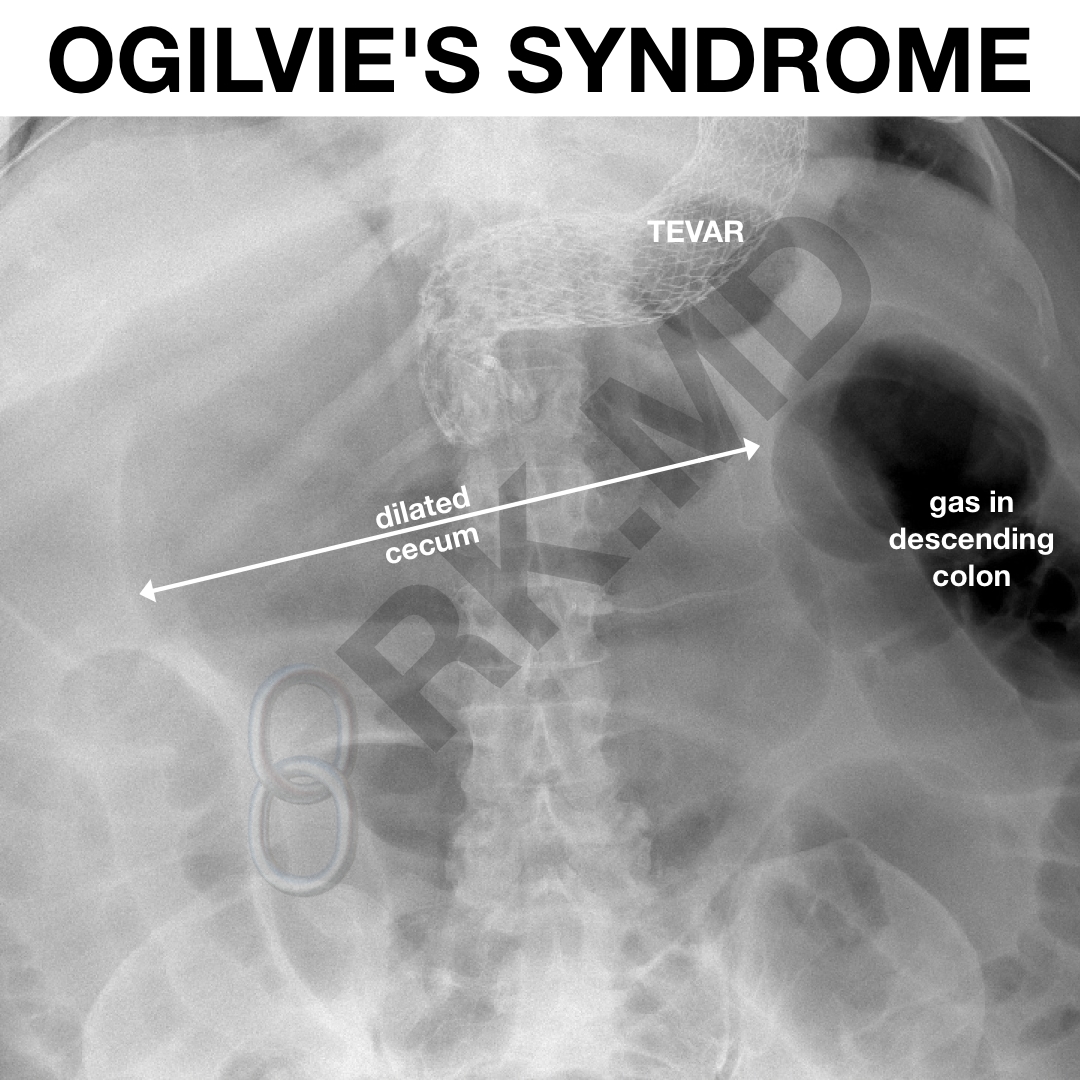
Ogilvie’s syndrome is an acute, paralytic ileus of the colon without mechanical obstruction associated with massive right colon dilation. Symptoms can include abdominal distension/pain, constipation, and in more severe situations, leukocytosis with fevers.
In line with Laplace’s Law (tension ~ intraluminal pressure * radius), since the cecum has the largest diameter of all colonic segments, its wall tension will also be the highest given increased pressure dispersed throughout the bowel. Therefore, cecal distension is often seen on abdominal x-rays (pictured), and if left unaddressed, can progress to ischemia, necrosis, and perforation.
The mechanism for Oglivie’s is attributed to autonomic dysregulation of the enteric nervous system (↓ parasympathetics, ↑ sympathetics). Risk factors include trauma, critical illness (sepsis, shock), infection, post-op status, and cardiac disease. As with many things in critical care, prevention is the best treatment – early ambulation and enteral nutrition, correcting electrolyte derangements, minimizing prolonged opioid use, and avoiding antibiotics that disrupt normal gut flora are all strategies to prevent Ogilvie’s.
If conservative measures fail and symptoms persist/worsen after a few days, one can pursue alternatives like neostigmine or intestinal decompression with NG/rectal tubes or endoscopically. Bowel perforation is associated with high mortality and requires a surgical intervention (bowel resection, diversion, etc.)
Drop me a comment below with your experience regarding Ogilvie’s syndrome!