Cardiac output (CO) is mathematically calculated as the product of heart rate and stroke volume. It’s related to preload, afterload, and contractility. One echocardiographic technique I routinely use to estimate a patient’s stroke volume is the volume-time integral (VTI).
The VTI method is based on the Doppler effect which relates to the perceived change in frequency of sound waves as they reflect off moving objects. Using a pulsed-wave Doppler (PWD) technique, I can identify the velocity of flow over time in a specific area (“sampling gate”), which for VTI-based CO will be in the left ventricular outflow tract (LVOT).
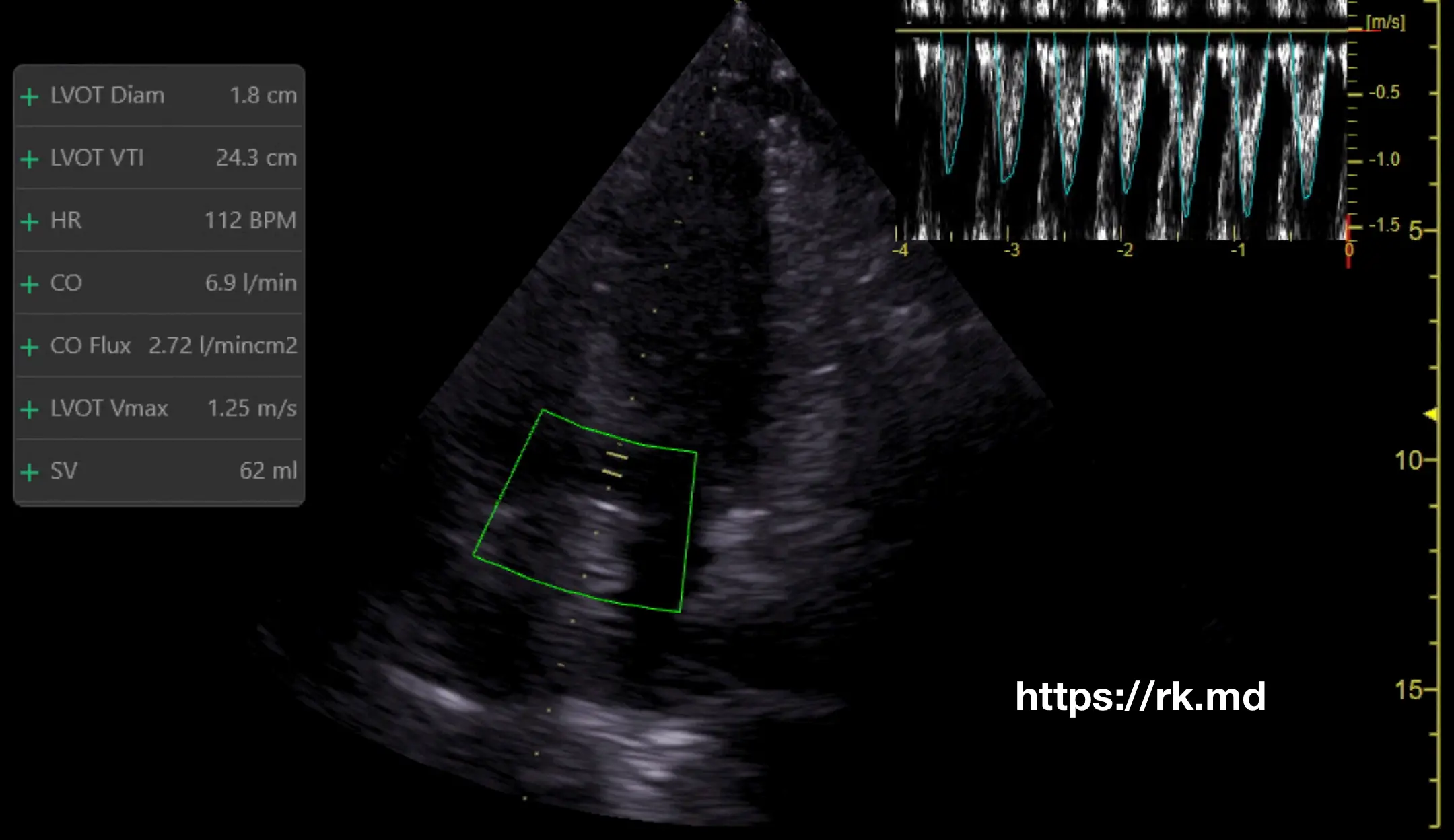
- First, I’ll acquire an apical five-chamber transthoracic echo view of the LVOT.
- Next, I’ll position the sampling gate in the LVOT and activate PWD to generate a spectral Doppler profile.
- I’m interested in forward flow exiting the LVOT into the aortic root during systole. As this flow is moving away from the transducer, this will be below the baseline.
- Next, I’ll determine the VTI by tracing the waveform envelope, which represents the peak blood flow velocity, and calculating the area under the curve.
- The blood vessel or cardiac chamber’s cross-sectional area (CSA) must be known to convert the VTI into volume. This can be estimated by measuring the LVOT diameter (d) in the parasternal long-axis transthoracic echo view. CSA = π x (d/2)2
- Multiply the VTI by the CSA to obtain the SV, representing the amount of blood ejected with each heartbeat. In other words: SV = CSA x VTI. After determining the heart rate from a monitor, CO = SV x HR.
I’ll use this technique in combination with a passive leg raise (PLR) to assess for fluid responsiveness. PLR results in an autotransfusion of blood from the periphery into the central circulation, and if this gets translated to an increase in VTI > 10%, I’ll consider fluid administration. That said, a normal VTI is ~18-22 cm in normal sinus rhythm.






Thank you