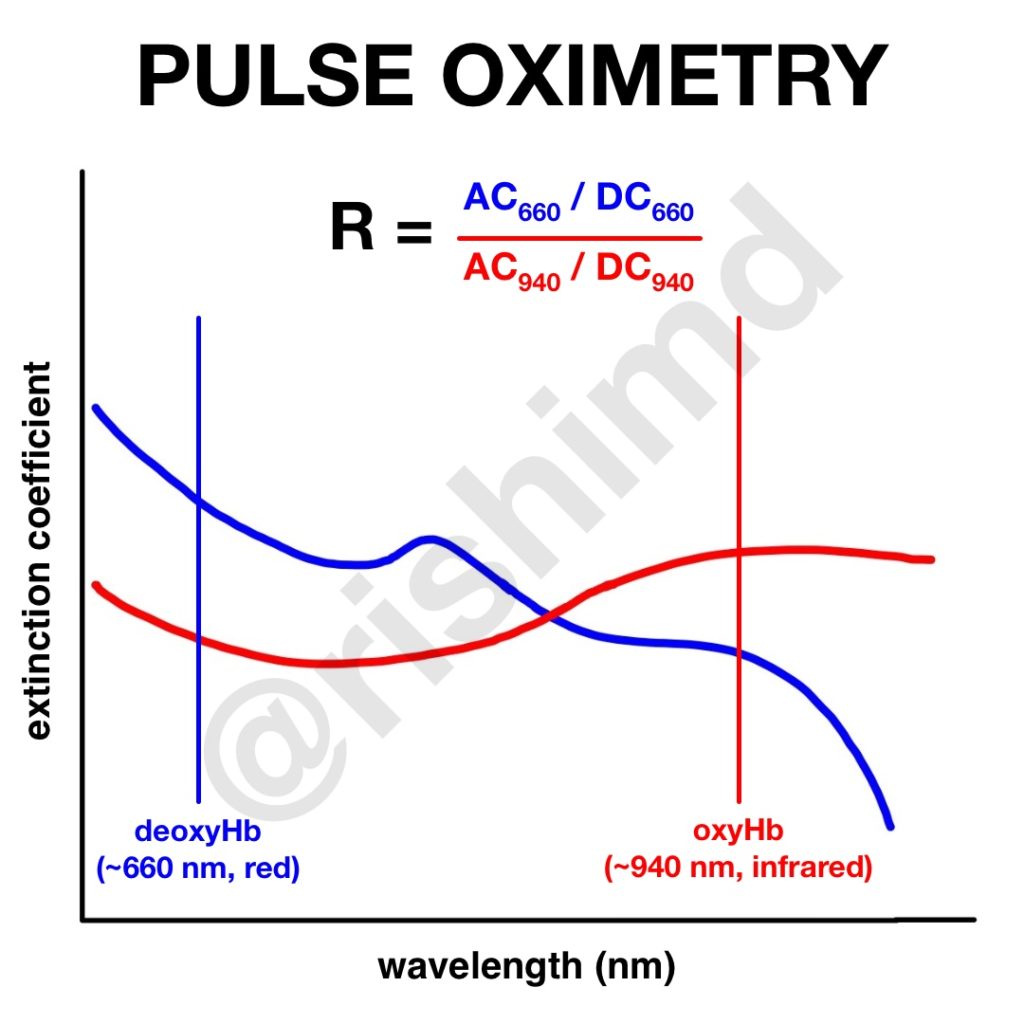
Routinely utilized in ICUs, operating rooms, and telemetry floors, the pulse oximeter (“pulse ox“) is perhaps the single greatest monitoring advancement in the modern medical era. It relies on the fact that oxyhemoglobin and deoxyhemoglobin absorb light at two different peak wavelengths. Without getting into too much detail, an algorithm is able to compare these ratios, exclude noise, and output an O2 saturation (SpO2).
What I want to clarify with this post is a misconception I’ve occasionally heard when interpreting the SpO2. A pulse oximeter does not measure the amount of oxygen in the blood. It only measures the degree to which a person’s hemoglobin is saturated.
CaO2 = (1.34 * [Hb] * SpO2) + (0.003 * PaO2)
CaO2 is the total arterial oxygen content, [Hb] is the hemoglobin concentration (from an arterial blood gas), SpO2 is the O2 saturation (from a pulse ox, expressed as a decimal), and PaO2 is the partial pressure of arterial oxygen (from an arterial blood gas). Clearly the SpO2 does contribute to the CaO2, but it certainly isn’t the whole story.
Your patient’s pulse ox can still read 100% even if their hemoglobin is 3 g/dL (critically low). In this case, the little hemoglobin they have is all saturated, but based on the CaO2 equation, their overall O2 content is extremely low. Take home message: SpO2 must be interpreted with the [Hb]!
If I know a patient is severely anemic (ie, hemorrhaging from penetrating trauma), they rely more on the undissolved oxygen (PaO2) to supply their overall content (CaO2). I’ll oxygenate these patients on close to 100% oxygen to maximize their PaO2 and ultimately CaO2 by the equation above until I catch up with resuscitation.
As a side note, if I could only have one monitor connected to my patient, it would be a pulse oximeter. With this noninvasive tool, we can ascertain the oxygen saturation of hemoglobin, the presence of distal perfusion due to a waveform, the heart rate, and even a rough idea of the heart rhythm. Pretty cool! 🙂






Great article. I have been utilizing the pulse ox perfusion index with a zoll X series monitor for a year now and have noticed interesting variability in many patient populations. There are expected low PI values in patients with low perfusion states (ie shock) but the “normal” values have a ton of variability–anywhere from 1-10. I’m not quite sure what to make of this variability.
It would be interesting to correlate these values with cardiac index or to quantify them in a meaningful way. Are you aware of any guidelines available to interpret these numbers?
Thanks for the comment, Tanner! Off the top of my head, I can’t think of any specific guidelines. I’ve seen pulse oximeters of different kinds placed on different sites of the same patient give remarkably different SpO2s… which can be concerning if you base treatment (oxygen therapy, ventilator settings, inhaled vasodilators, etc.) off of a number. Often times I see how a patient’s PaO2 on their ABG correlate with the SpO2 to see if it’s what I’m expecting (ie, a PaO2 ~ 60 mmHg should have an SpO2 of around 90%). Here’s an article that discusses that: Correlation between the levels of SpO2 and PaO2
It’ll be interesting to see what the next generation of monitors brings in terms of accuracy/precision! 🙂
Thank you for the article recommendation!
I’ve been reflecting on this paragraph from your lesson: “If I know a patient is severely anemic (ie, hemorrhaging from penetrating trauma), they rely more on the undissolved oxygen (PaO2) to supply their overall content (CaO2). I’ll oxygenate these patients on close to 100% oxygen to maximize their PaO2 and ultimately CaO2 by the equation above until I catch up with resuscitation.”
Do you have a specific hemoglobin number that you use when implementing hyperoxygenation? And are you ever concerned about O2 induced coronary vasospasm in an anemic patient with, say, an occlusion MI or the like?
No specific number. It’s a temporizing measure while resuscitating with blood products. And in those dire circumstances, I’m less concerned about the well known risks of hyperoxygenation (ie, free radical damage) and more worried about the systemic effects of low O2 delivery. The latter will arguably result in more acute/hyperacute problems.
Well, quite an intersting article…. Had a discussion with a colleague earlier this month about SpO2 and EtCO2…. If you had to choose btw the two, which one would you go for? I’d definitely go with pulse ox as far as I’m concerned…. What about you?
I’ll definitely take the pulse oximeter as well. Besides being more useful, in my opinion, I feel like other care providers (nurses, techs, etc.) are more familiar with a pulse oximeter compared to a ETCO2 monitor.