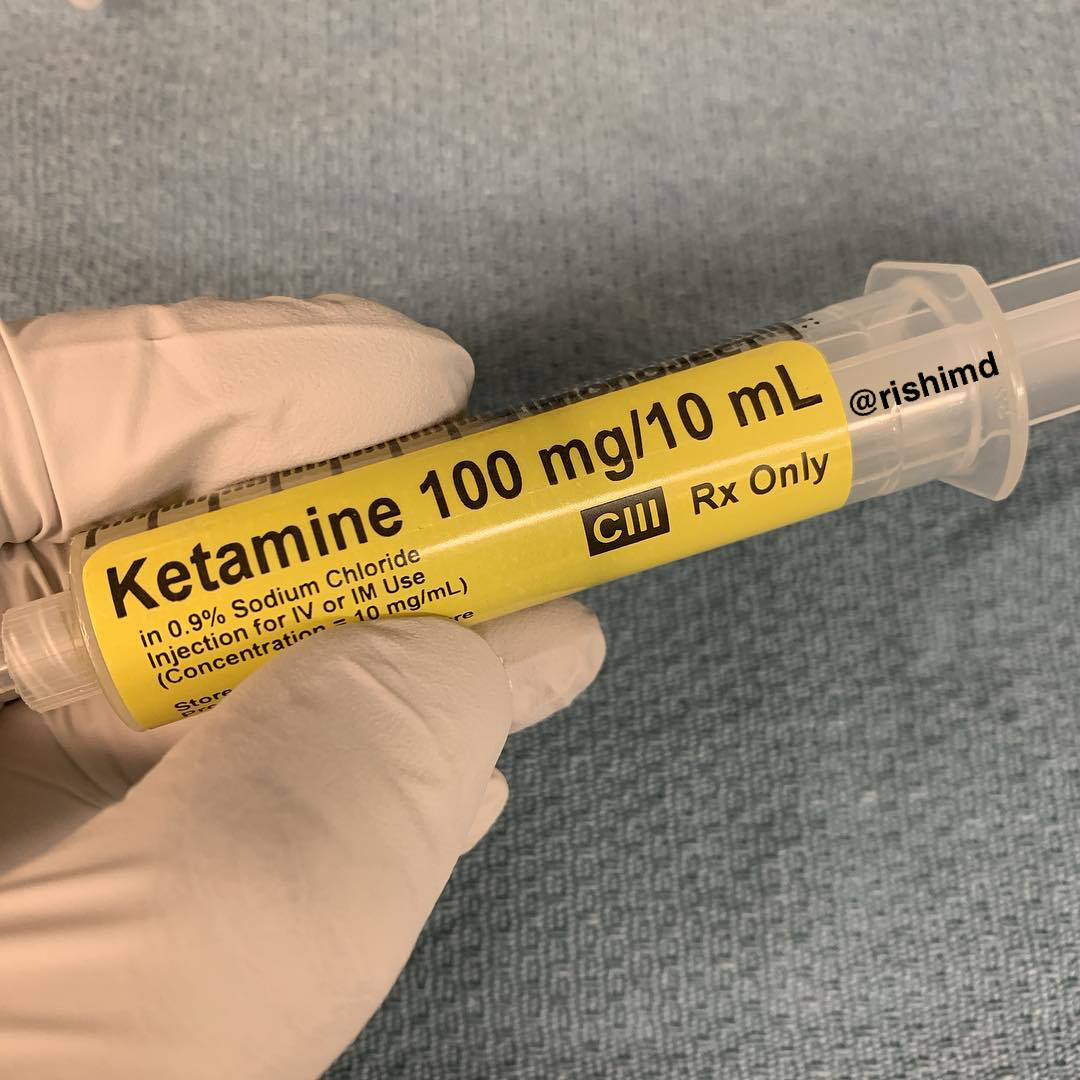
Ketamine (Ketalar) is my FAVORITE medication in perioperative and critical care medicine! It’s a unique dissociative amnestic, an almost complete anesthetic in itself, has tremendous versatility in terms of routes of administration (IV, IM, oral, subcutaneous, intranasal, sublingual, rectal, epidural, transdermal), and unique properties as an analgesic and antidepressant!
Ketamine is an NMDA receptor antagonist – in other words, it blocks the “excitatory” glutamate molecule from binding this receptor forcing it to bind other receptors like AMPA and kainate and increase structural synaptic connectivity. This is a proposed mechanism behind how ketamine infusions work in treatment refractory depression (TRD). It has several proposed mechanisms for analgesia, namely inhibition of the NR2B NMDA subunit, opioid potentiation through delta opioid receptor activation, potential dopaminergic modulation, and nitric-oxide synthase inhibition.
Although ketamine is a myocardial depressant, it’s sympathomimetic effects tend to compensate thereby preserving hemodynamics. Additionally, ketamine is a potent bronchodilator (although it increases secretions). In general, I think we underutilize ketamine because of a.) unfamiliarity with the medication and b.) psychotomimesis (hallucinations/delirium), the latter being used for recreational purposes (“Special K”).
I advocate for residents who work with me to use ketamine (in appropriate cases/patients) and learn how to manage its side effects (ie, short acting benzos for delirium). One strategy I often use for long, painful surgeries in patients with a chronic pain syndrome is a combo lidocaine/ketamine drip (20 cc of 2% lidocaine, 1 cc of 100 mg/cc ketamine) in a pump syringe and run it at 1 mg/kg/hr of lidocaine (which will also deliver 0.25 mg/kg/hr of ketamine). I’ll turn this infusion off 30 minutes before emergence.
Drop me a comment below with questions! 🙂






Hi Rishi,
That was a great post. I was wondering how you would run an RSI- Like would you choose Rocketamine – or Ketofol or any other combination ?
The overwhelming majority of my RSIs in the ICU consist of propofol, high dose rocuronium, and push dose pressors (dilute norepinephrine, epinephrine, etc.)
Hi Rishi
Thank you for a great post. When benzodiazepines can be used to prevent delirium from Ketamine, would you still consider giving midazolam for instance for patients above 70 yo ? If so do we need to take it to the account whether it is a general or a MAC ? Thank you for your time.
I don’t routinely administer midazolam to prevent delirium from ketamine, and I find myself using very subanesthetic doses as an adjunct for pain.