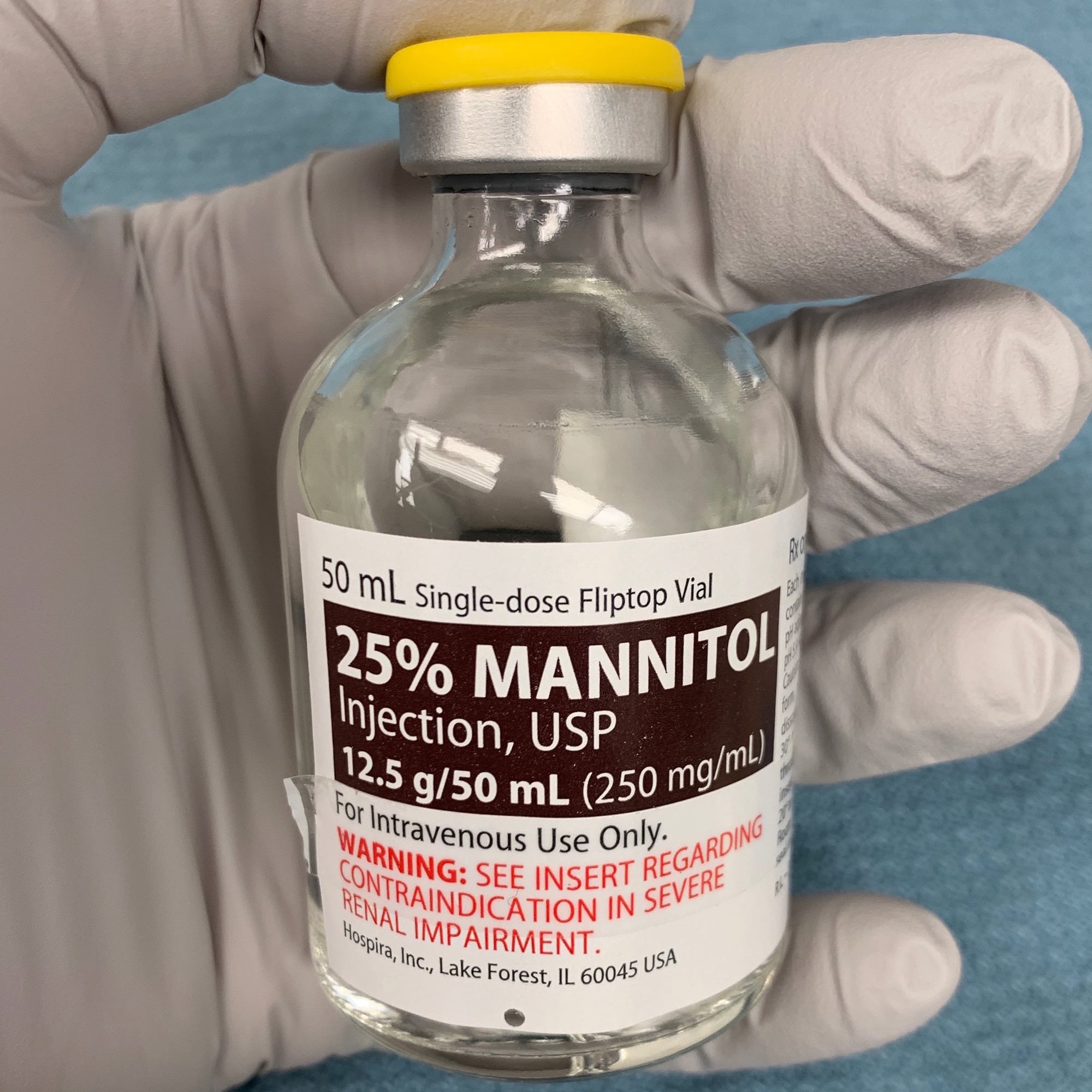
Mannitol is a carbohydrate often administered as a hypertonic solution that is freely filtered by the renal glomerulus and not reabsorbed. Therefore, it serves as an osmotic diuretic that, if left unchecked, can lead to electrolyte derangements and hypovolemia.
As an intensivist, I most commonly use mannitol to treat acute increases in intracranial pressure (ICP) measured with an external ventricular drain or bolt. As a cardiac anesthesiologist, I sometimes use mannitol (with Lasix) on cardiopulmonary bypass to augment urine output and during renal transplants prior to vascular clamp removal to decrease allograft injury by improving perfusion and free radical scavenging.
In either case, one must consider the ACUTE INCREASE IN INTRAVASCULAR VOLUME created with mannitol. If a patient cannot mobilize this additional fluid (ie, compromised cardiac function), they may be thrown into acute congestive heart failure which can cause fluid to back up in the systemic and/or pulmonary circuits. Additionally, pre-existing renal injury can cause mannitol to be retained in the blood stream leading to consequences of hyperosmolality (hyponatremia with possible neurologic sequelae, hyperkalemia with dilutional acidosis, etc). Always weigh the pros and cons!
Drop me a comment below with questions! 🙂