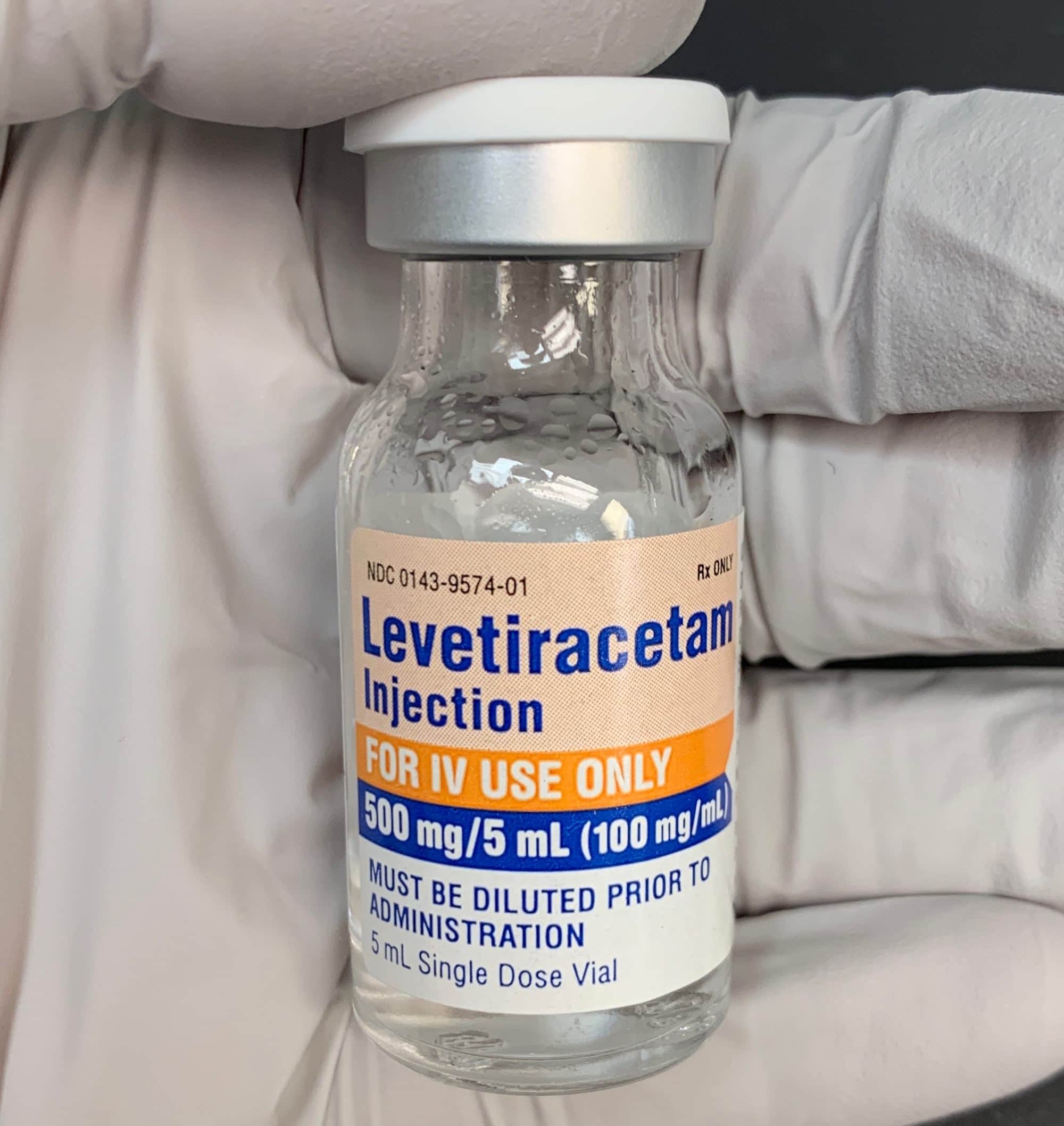
Levetiracetam (Keppra) is an oral and intravenous antiepileptic drug (AED) indicated as adjunctive therapy for partial onset seizures, myoclonic seizures, and generalized tonic-clonic (“grand mal”) seizures in adults. The medication is used in the pediatric population as well for various reasons beyond my scope of practice. Most AEDs either enhance the release or limit the uptake of GABA – the primary inhibitory neurotransmitter in the central nervous system. Levetiracetam’s activity is thought to center around SV2A, a ubiquitous synaptic vesicle protein involved in regulating the exocytosis of neurotransmitters from vesicles.
Post-traumatic seizures (PTSs) are fairly common in patients who sustain traumatic brain injuries (TBIs), and the early initiation of AEDs like phenytoin help decrease early PTS in severe TBI; however NO AED prophylaxis I’m aware of helps prevent late TBIs. Lower levels of data suggest that newer AEDs like levetiracetam may be a safer alternative to phenytoin for early PTS prophylaxis.
As an anesthesiologist, I can’t remember when I last administered levetiracetam intraoperatively (general anesthesia tends to be a pretty good antiepileptic itself), but as an intensivist, I’ve written for this many times at the recommendation of my colleagues in neurology. Interestingly, the oral formulation of levetiracetam is ~100% bioavailable, and its renally-excreted metabolites have no activity.
Regardless of why it’s given, levetiracetam can increase the risk of suicidal ideations (even within a week), so providers must remain vigilant about any unusual changes in mood or behavior in patients initiated on therapy.
Drop me a comment with questions! 🙂