We’ve all seen “type and screen” orders, but what does a blood type tell us?
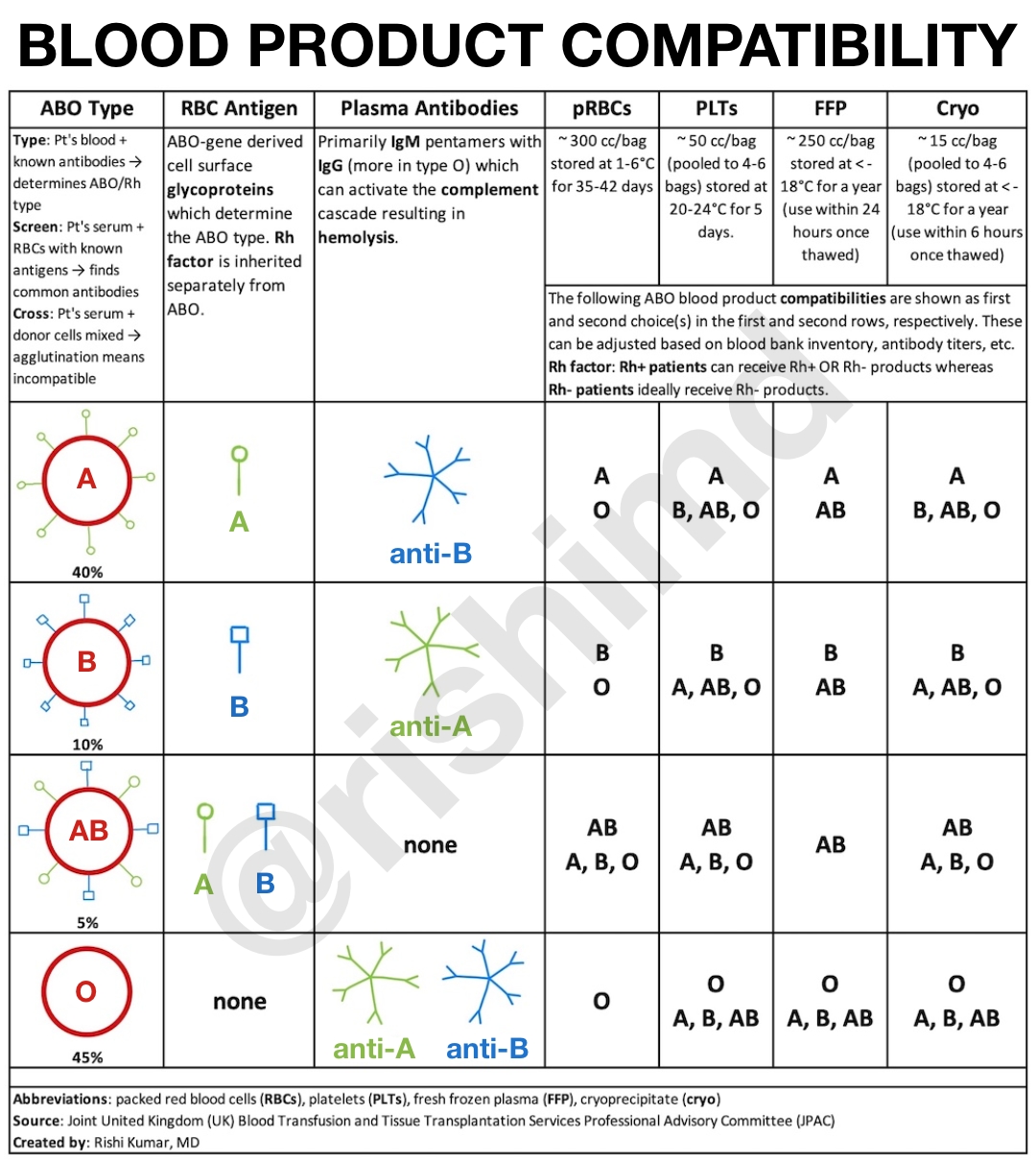
ABO grouping refers to the surface antigens on our red blood cells (RBCs). For example, type A RBCs have A antigens on their surfaces, type B RBCs have B antigens on their surfaces, and type O RBCs have neither A nor B antigens.
Now, one must consider the resulting antibodies in the plasma. For example, patients with type A blood have anti-B antibodies in their plasma. This makes sense because if they had anti-A antibodies, they would attack their surface antigens resulting in hemolysis. This concept is how we determine compatible blood transfusion options for patients.
Let’s look at fresh frozen plasma (FFP) donated by someone with type O blood. Although their RBCs are devoid of A and B antigens, their plasma contains anti-A AND anti-B antibodies. Therefore, a transfusion reaction will likely occur if this plasma is transfused into a patient with either A or B surface antigens (ABO types A, B, or AB). This is why although type O is considered a “universal RBC donor,” type AB is a “universal plasma donor,”… although they would technically need to be Rh-.
Keep in mind that this simplified table does not illustrate all the details (e.g., Rh/anti-D) or consider titers, blood bank inventory, etc.
Drop me a comment with questions and if you found the table helpful! 🙂






Can you talk about estimated blood loss and how you calculate this value in the OR. and what is your method for replacement with both blood product, crystalloid, & colloid
Clinical judgment.
EBL is difficult to gauge in the OR cases I’m involved with due to blood salvation techniques. I’ll use a combination of monitors, echocardiography, visual cues (how does the heart “look” in the field), etc. combined with labs (hematocrit) and other issues (coagulopathy, RV dysfunction, etc.) to determine what kind of fluid and how much to administer.