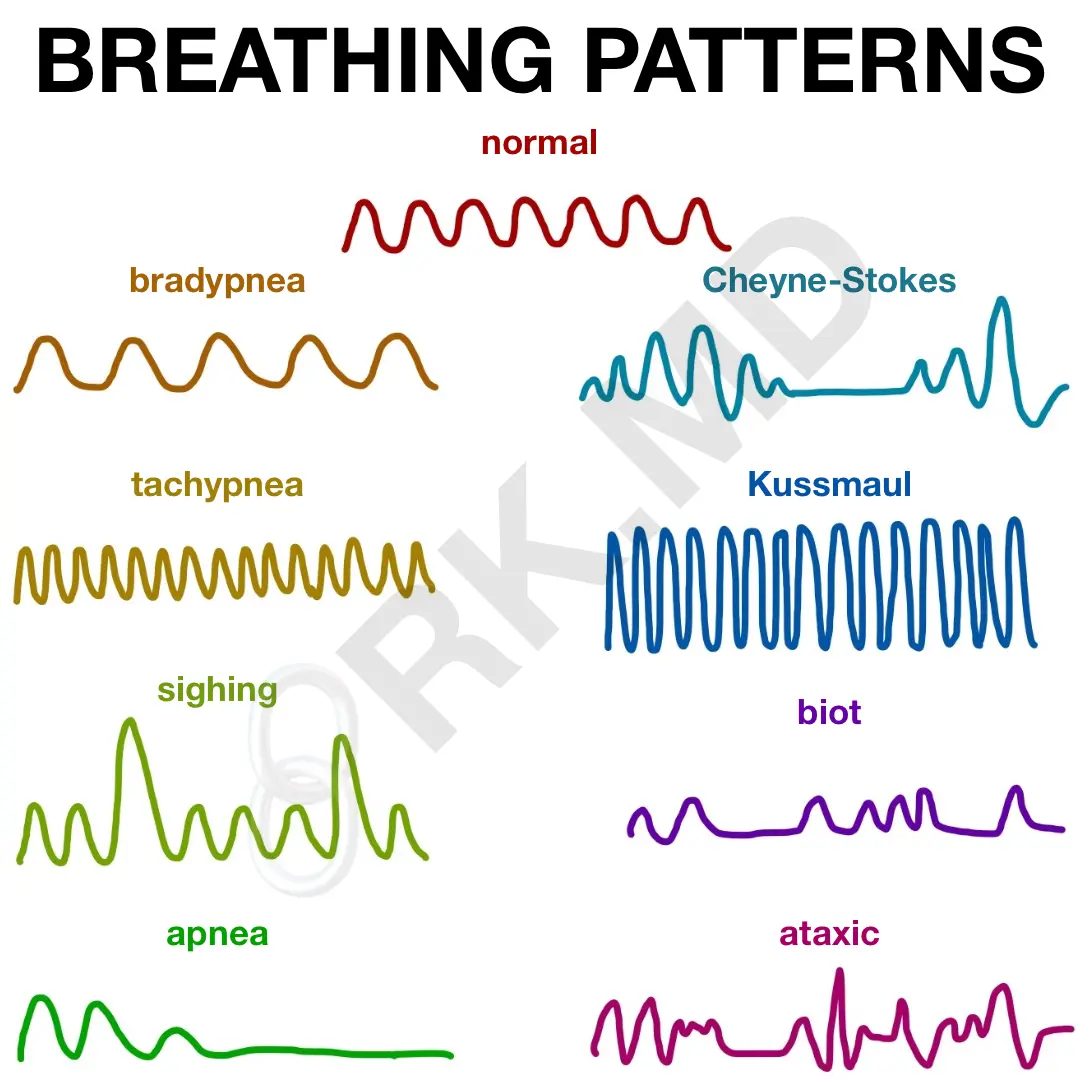
A patient’s breathing pattern can help guide response to therapies and diagnostics. Normal breathing is regular and comfortable at a rate of 12-20 breaths per minute (bpm).
Tachypnea and bradypnea have rates above and below that range, respectively. Tachypnea can suggest a normal response to exercise, pain, sepsis, metabolic acidosis, PE, COPD, congestive heart failure, pain, anxiety, etc. In comparison, sepsis, pain (splinting), and central nervous system (CNS) depression from trauma or medications (i.e., oversedation) can result in bradypnea.
Sighing, on average, occurs once every five minutes and helps with alveolar recruitment. Snoring with intermittent apnea may suggest OSA.
Cheyne-Stokes is characterized by waxing and waning tachypnea with interposed apnea and suggestive of various pathologies ranging from heart failure with pulmonary edema to severe CNS injury or even uremia. 😷
Kussmaul breathing is classically associated with diabetic ketoacidosis and seen as deep and rapid respirations. With an injury to the medulla oblongata, one may see an irregularly irregular pattern of equal depth breathing with intermittent apnea known as biot breathing. This can progress to total irregularity in breathing intervals and depths known as ataxic breathing.
Drop me a comment below with questions!