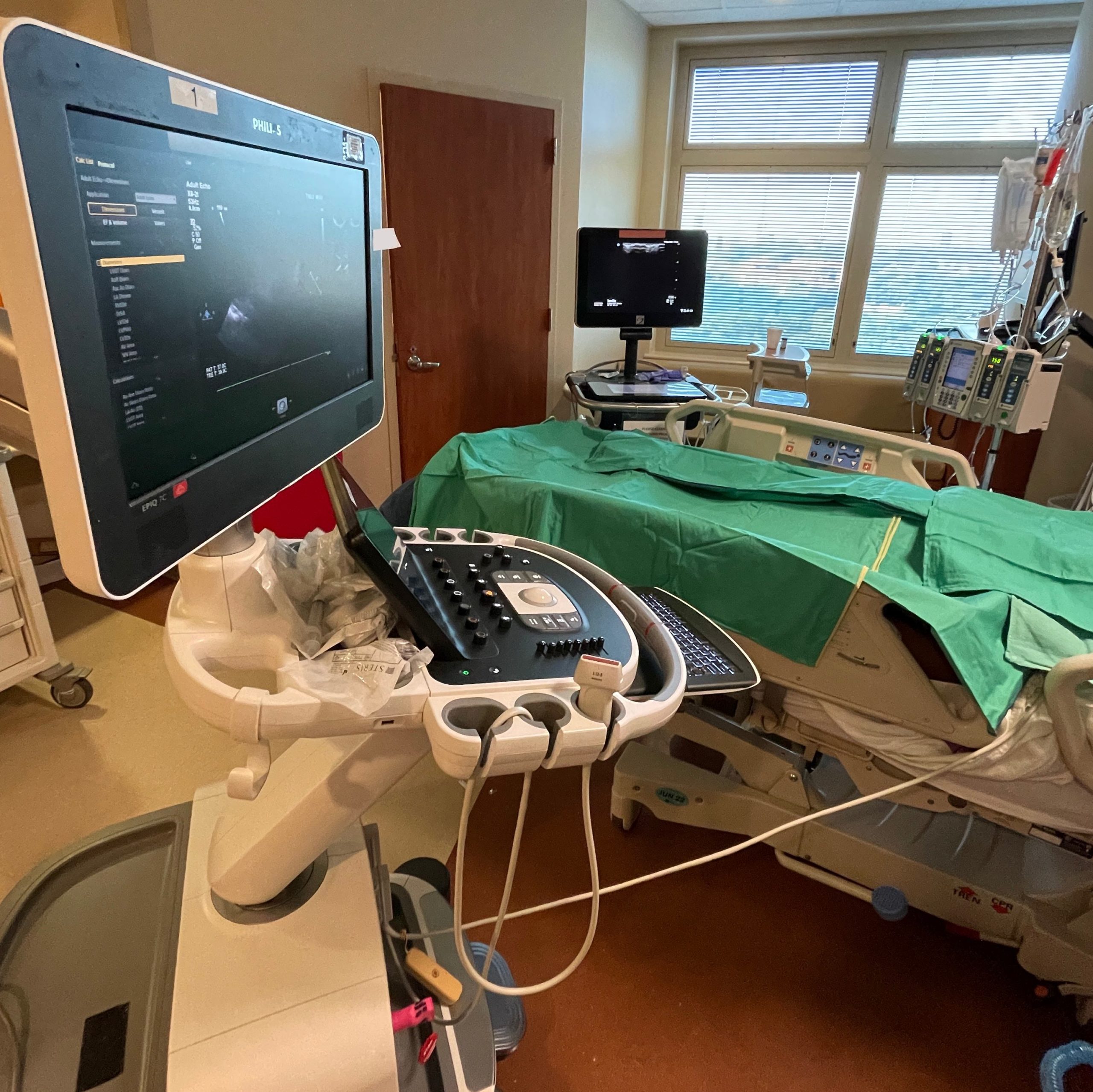
As a cardiothoracic (CT) intensive care unit (ICU) physician, knowing how to balance resuscitation with inotrope and vasopressor support is a large part of my job. For patients on post-operative days (POD) 0 or 1, typical bedside ultrasound views are challenging to come by due to sternal dressings, chest tubes, air in the chest, etc.
Instead, I’m a firm believer in the diagnostic power of transesophageal echocardiography (TEE) in unstable patients in the ICU. Not only does this modality give me a real-time assessment of valvular and biventricular function, but it also allows me to dynamically assess response to therapies. I use TEE in combination with continuous cardiac output monitoring, mixed venous oxygen saturation, pulmonary artery pressures, and systemic arterial pressures to determine how to best intervene and assess for new problems that may develop post-operatively (i.e., extracardiac clots causing tamponade).