To maximize gas exchange, well-ventilated alveoli (V) should be associated with good pulmonary capillary blood perfusion (Q). This is the idea behind V/Q matching. Gravitational forces create heterogeneity perfusing dependent portions of the lung better – the lung base in the upright position, and the posterior lung in the supine position.
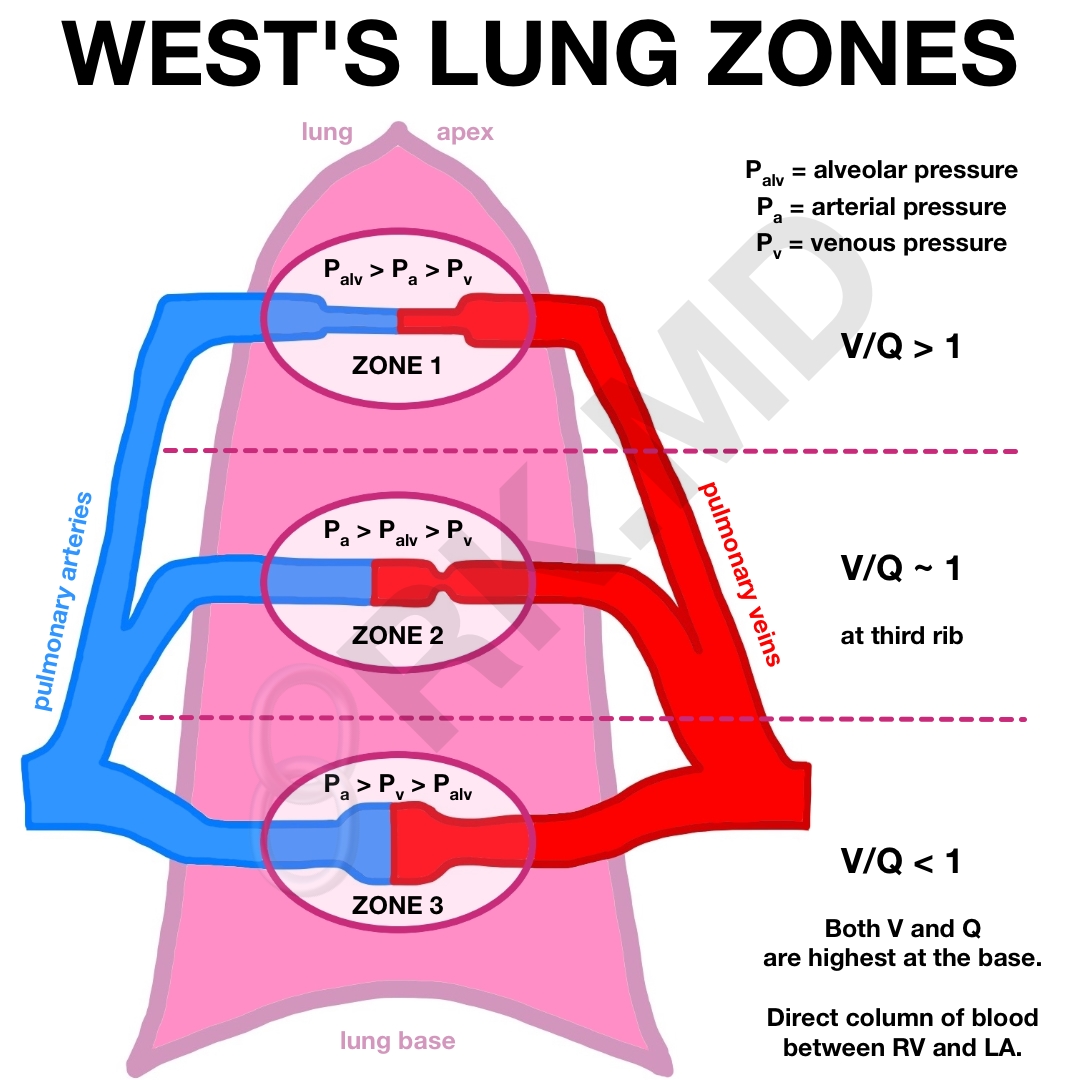
West’s Zones divide the lung into regions where pressures in the pulmonary arteries, veins, and alveoli determine flow through the pulmonary vasculature. In zone 1 (apex of the upright lung), Palv exceeds vascular pressure leading to areas of collapse (ventilation without much perfusion = dead space). In zone 2, the flow depends on a balance between arterial and alveolar pressure. In zone 3, vascular pressures (both arterial and venous) exceed that of the alveoli. Since there isn’t any collapse in zone 3, there’s a direct column of blood connecting the right ventricle and left atrium.
Because of this smooth transition of blood in zone 3, this is where we want our PA catheters to be positioned to estimate left-sided heart pressures. Fortunately, in the SUPINE position, most of the lung is considered zone 3.
Drop me a comment below with questions! 🙂






Thanks for this awesome explanation!
You’re very welcome!