As a cardiac anesthesiologist and cardiovascular intensivist, I routinely care for perioperative cardiac surgery patients in my OR and ICU practices. If I were to look at the “I&Os” (intake and output) to estimate how “net positive” a patient is for their hospital admission without breaking down the types of fluids, I’d be misled.
For example, not all intake is created equal. Enteral intake (tube feeds, free water flushes, etc.) differs from parenteral intake (IV fluids, TPN, IV antibiotics, etc.). Furthermore, not all parenteral fluids are equal – the body will handle 500 ccs of packed red blood cells differently than 500 ccs of crystalloid.
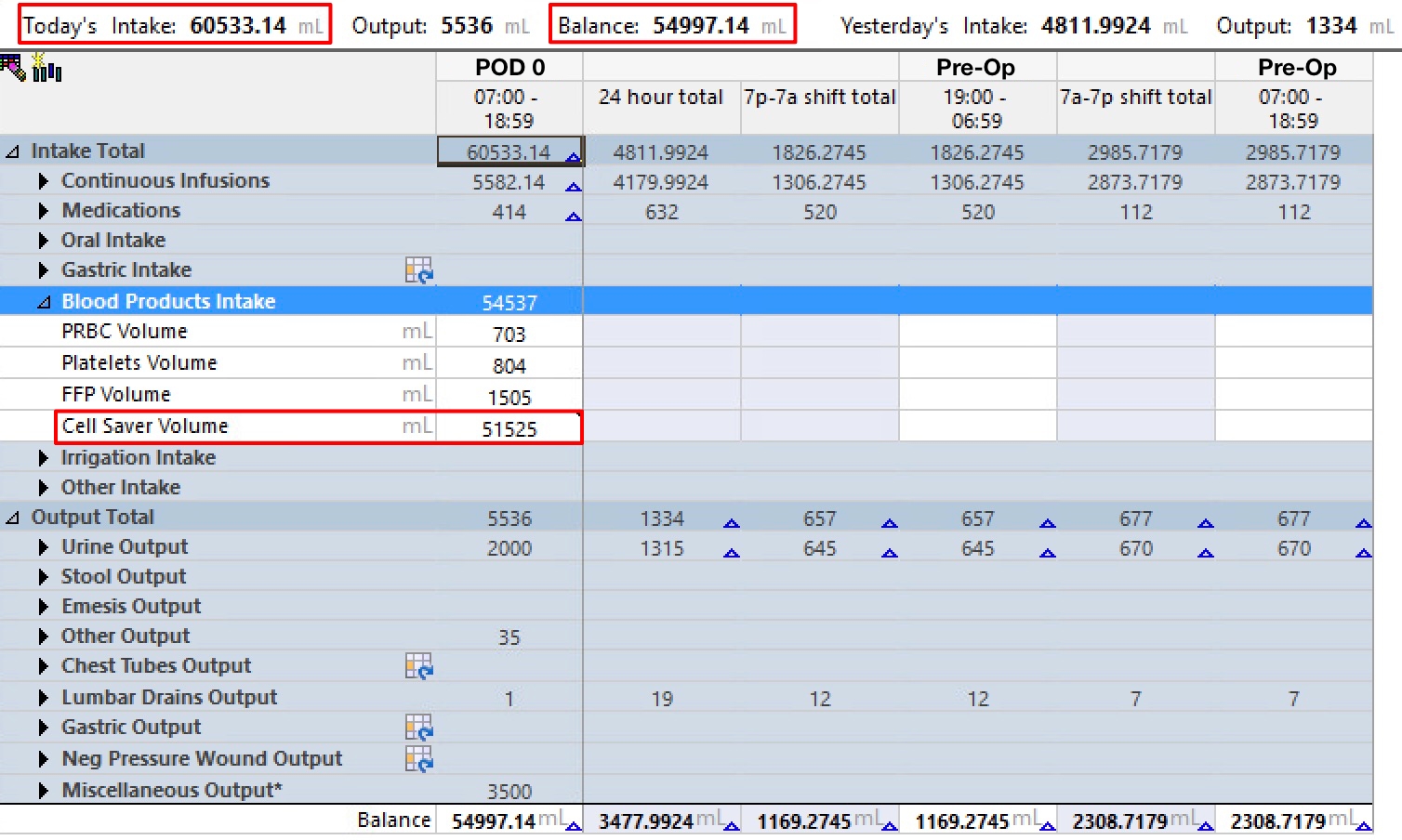
Cell Saver is comprised of red blood cells that is autotransfused back to the patient; however, it’s charted as an intake just like crystalloids, albumin, etc. Extent II open thoracoabdominal aneurysm repairs routinely involve transfusing large amounts of Cell Saver intraoperatively; however, on the ICU side, this cannot be counted as a net 50+ liters of intake (see the example) since this is blood that is leaving the patient’s body and being transfused back.
Several days later, the patient’s “Balance” will still be markedly positive because of how this is charted. Fluids should not be withheld based purely on one number in the chart – understanding the types of fluids and the bedside assessment of fluid status/responsiveness/tolerance are essential to critical care.