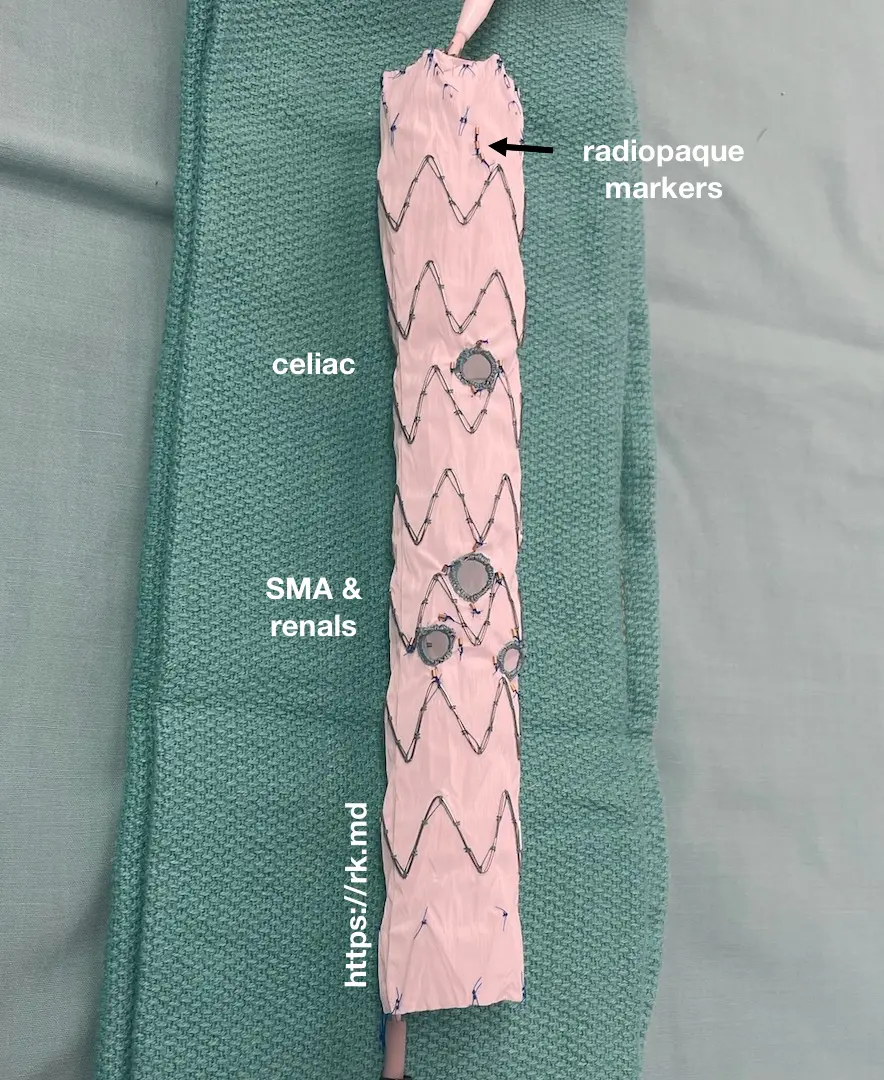
Physician-modified endovascular grafts (PMEGs) offer a percutaneous and effective option for repairing complex thoracoabdominal aortic aneurysms. A stent graft is modified onsite using strict sterile technique with reinforced fenestrations created based on the patient’s specific anatomy. Additionally, radiopaque markers are added to help with stent graft alignment in vivo. In addition to sealing the diseased aorta with the main body of the stent graft, these fenestrations allow vascular surgeons to address pathology associated with the renal or visceral vessel. This technique is called a fenestrated endovascular aneurysm repair (FEVAR).
After preparation, the stent is moved to a hybrid operating room, oriented extracorporeally, and introduced into the patient’s aorta via a sheath in the femoral artery. Using sophisticated imaging and software, the live fluoroscopy image is fused with the patient’s prior CT angiogram – this allows the surgeon to know the location of the visceral vessels without constantly needing to do angiograms. The vessels are cannulated, the main stent-graft is deployed and reinforced with balloon dilation, and additional stent-grafts are placed within the fenestrations to maintain patency to the celiac artery, superior mesenteric artery (SMA), and bilateral renal arteries in the pictured PMEG. Imaging is performed to assess for endoleaks, technical defects, and vessel patency before leaving the operating room.
I want to thank the amazing vascular surgery trainees for supplementing my understanding of this topic with their knowledge and experiences.