Today marks the end of my first year of clinical anesthesia (CA-1) and wanted to reflect on things I learned. While my intern year was filled with lessons inherent to becoming a new physician, my CA-1 year was very different! Anesthesiology has an incredibly steep learning curve – advanced physiology and pharmacology, new terminology, procedural skills, and nuances to different anesthetics (ie, a cardiopulmonary bypass case is very different than a cerebral aneurysm repair) made this year challenging yet fulfilling.
COUNTLESS RECIPES
Every attending has a slightly different anesthetic plan for the same case, and most think their way is the “right way.” As a trainee, this can often be frustrating as it’s hard to learn a single approach for a given case; however, this is the awesome part of anesthesiology! Take some of the good techniques, leave the bad, and make your own recipe!
I’ve significantly changed the way I do general anesthetics from my first month and with much better results. Patients tend to emerge smoother and quicker than before with a more comfortable post-operative course in the PACU. As I’ve matured as a resident, I feel attendings give me more leeway with my intraoperative management and don’t nit-pick as much. 🙂
ANTICIPATE, THINK, ACT
Anesthesiology is a wonderful blend of troubleshooting changes in homeostasis. Managing fluid deficits, systemic hypertension, the stress response to surgery, vasodilation from neuraxial anesthesia, post-operative nausea/vomiting, bradycardia during laparoscopy, and the like are all incredibly common facets of anesthetic care. Many times, we have to diagnose problems based purely on subtle hints while the patient is unconscious. What does the urine look like? Are the surgeons creating an intense stimulus? Is the patient catecholamine-depleted? Why did the patient get tachycardic and hypotensive? Why did I lose my end-tidal carbon dioxide reading?
The patient can rarely tell you the answer. Assimilating the overall clinical situation is vital in diagnosing and treating the patient. Many times we can anticipate large changes in homeostasis (ie, Mayfield head pinning and an exsanguinating trauma patient) and act accordingly. Prevention is often the best form of treatment.
EMBRACE THE ROLE OF THE UNSUNG HERO
3 years of college + 4 years of medical school + 2 years of residency, and my official title, despite informal introductions, remains: “Hey you… anesthesia!” Patients rarely remember their anesthesiologist especially if everything is uneventful. We spend an extraordinary amount of time directly with our patients, but only a portion while they’re still awake. This puts us in the back seat as an unsung hero in the operating room… someone carefully watching over the patient while they endure a surgery. Don’t expect any credit, but expect to have the room turned over quickly or be victim to the all-too-common phrase: “anesthesia delay!” 😀
Going into my CA-2 year, I’ll be rotating through chronic pain, critical care, cardiothoracic anesthesia, pediatric anesthesia, neuroanesthesia, obstetric anesthesia, regional anesthesia… yeah… lots of anesthesia. 😀 I’m hoping the skills I learned (and more importantly, the mistakes I’ve corrected) will serve me well over the next year! 🙂
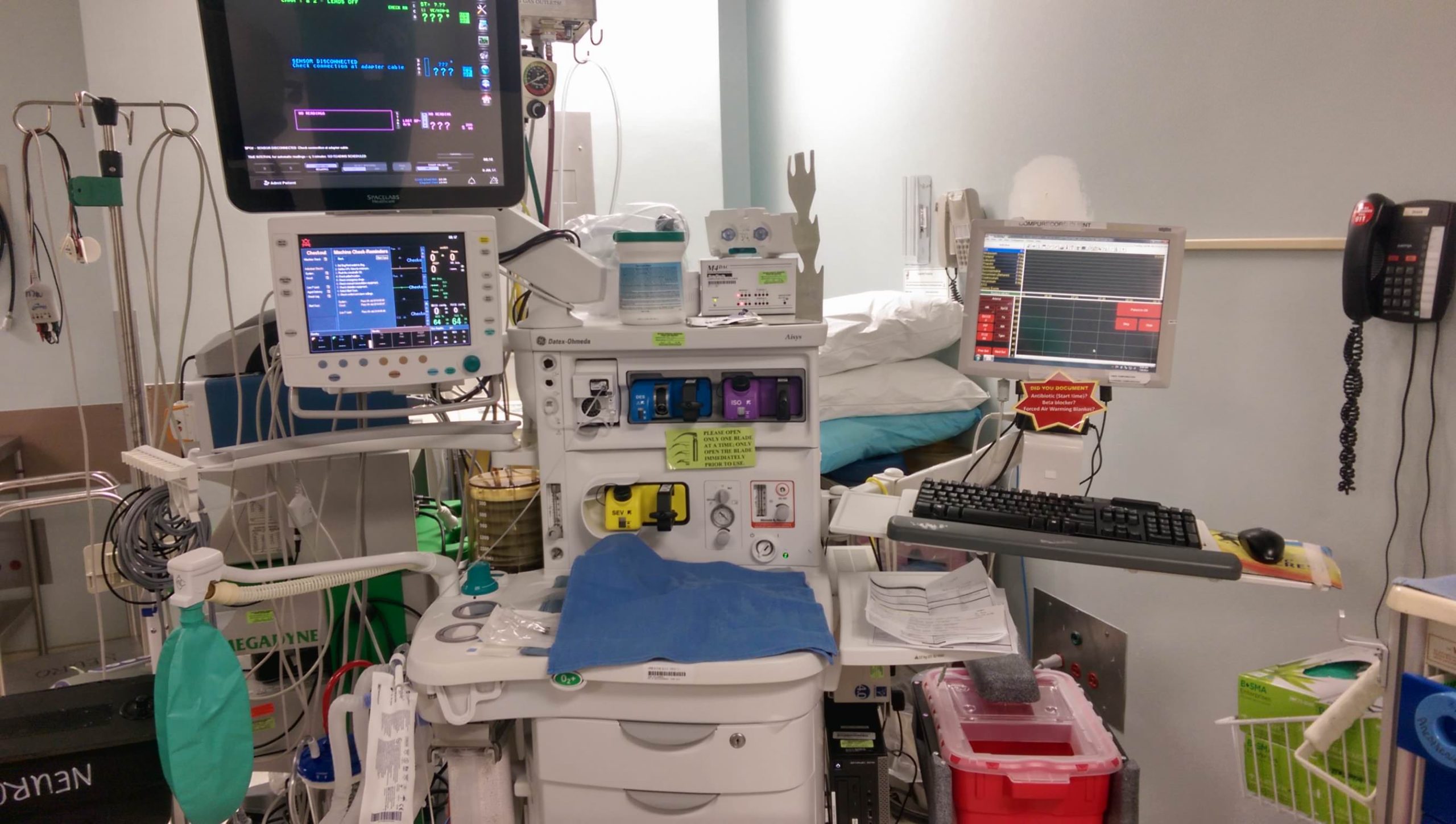
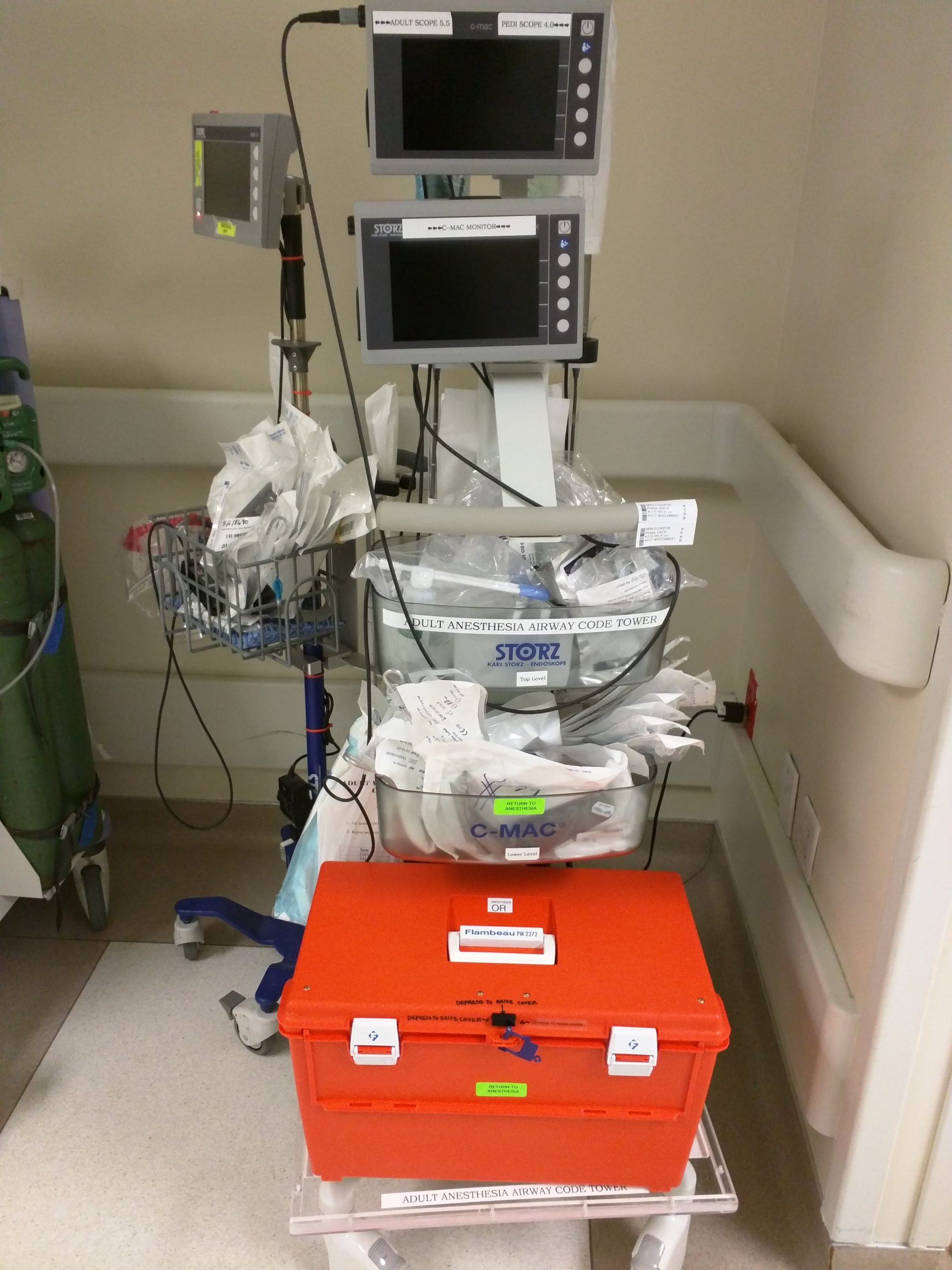
Now for some pictures from my first year of training: