Lactic acid fermentation is generally thought of as a process related to anaerobic metabolism in the context of tissue hypoxia from inadequate oxygen delivery and/or uptake. This “Type A” lactic acidosis is routinely seen in shock and states of high oxygen consumption (seizures, shivering, etc.)
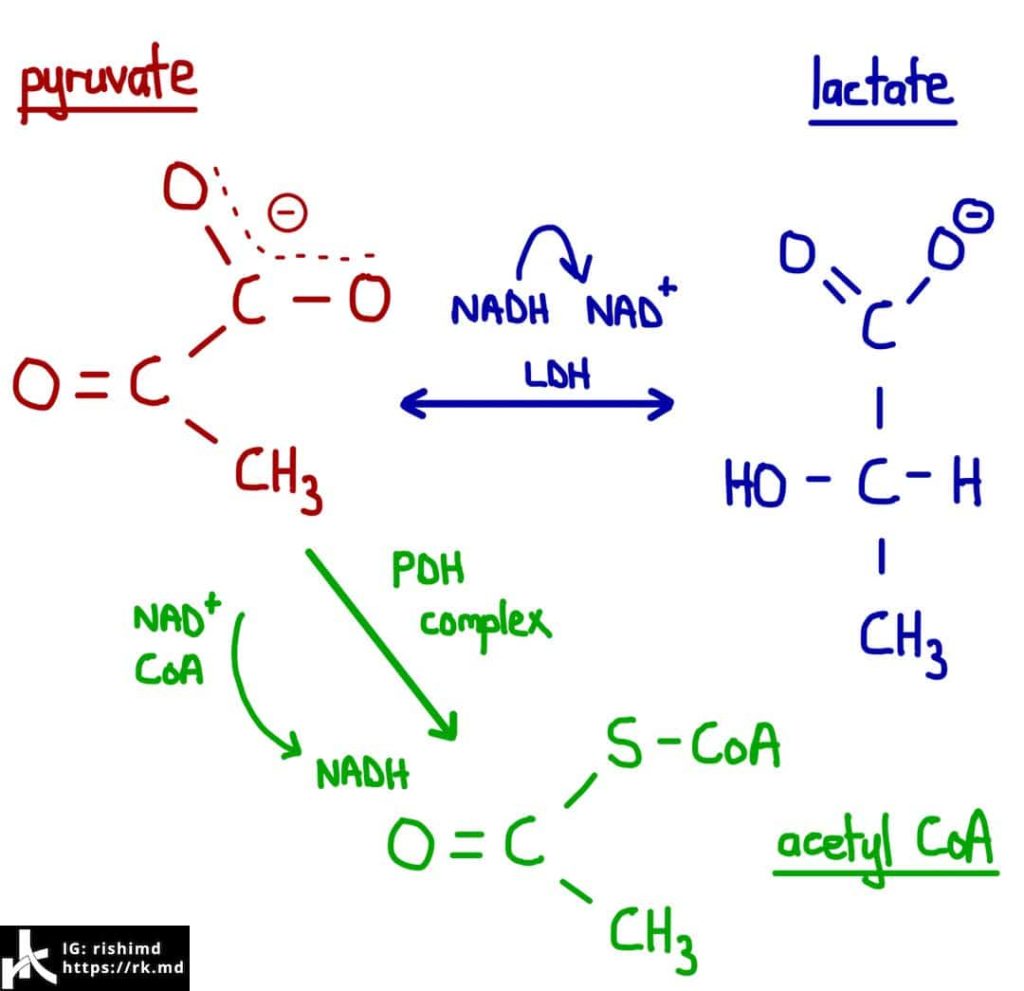
Remember that glycolysis is the first step in producing ATP – our cellular energy currency – and takes glucose through a series of steps to produce NADH and pyruvate. Under aerobic conditions, this pyruvate serves as a substrate for the pyruvate dehydrogenase complex (PDC) which ultimately generates the bulk of ATP by oxidizing high energy substrates in the Kreb’s cycle and electron transport chain (ETC).
Pyruvate can also undergo fermentation to oxidize NADH back into NAD+ while becoming lactate. Lactate serves as a fuel which, in turn, can undergo gluconeogenesis in the liver (Cori cycle). When the PDC is overwhelmed by high concentrations of pyruvate, much of this substrate is fermented to continue energy production. This is known as “type B” lactic acidosis and is seen routinely with medications, toxins, TPN, epinephrine, liver disease, and malignancies. This often presents as an up trending lactate in an otherwise stable-appearing patient. Always consider the possibility of ongoing ischemia before attributing an elevated lactate to a “type B” etiology!
Even under aerobic circumstances, we all generate some lactate each day. Problems arise when an increase in lactate production is coupled with a decrease in lactate metabolism (hepatic/renal insufficiency) as this can result in acid-base derangements with systemic effects.





