As an anesthesiologist, I’ve placed nasogastric/orogastric tubes (NGTs/OGTs) in patients who will remain intubated post-operatively to decompress the stomach and to provide a short-term enteral route of administration while the patient remains on mechanical ventilation. As an intensivist, I more commonly place NGTs to deliver nutrition (i.e., tube feeds) and medications in patients with impaired swallowing (a complex mechanism!)
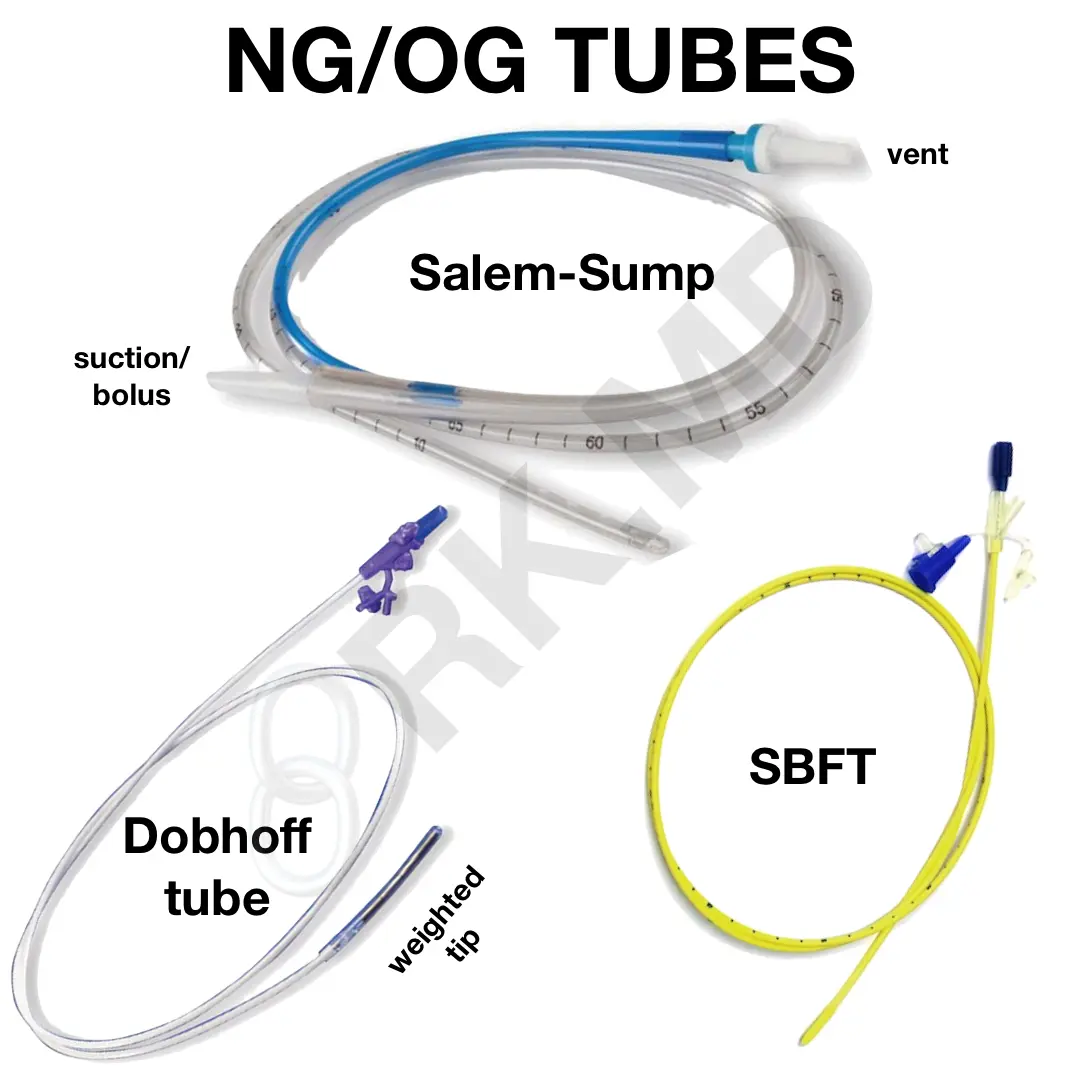
The Salem-Sump is a relatively large bore (10 – 18 French) dual-lumen tube which permits suctioning of gastric contents as well as medication/nutrition delivery. One port allows for wall-suction drainage or administration of therapy often facilitated with a Lopez valve. The other port is the sump vent, which equalizes gastric and atmospheric pressure (do NOT apply suction to this).
In comparison, traditional small bore feeding tubes (SBFT, i.e., Corpak) and Dobhoff tubes (named for the two physicians who created it – Drs. DOBbie and HOFFmeister) are smaller and more flexible, permitting a greater degree of comfort for the patient. These tubes contain an inner stylet that facilitates placement and is removed before usage. Due to the much more pliable material and smaller lumens, these tubes aren’t designed for suctioning and should only be used to administer tube feeds/medications.
Drop me a comment below with your experience regarding NGTs!






Can juven be given via dht
What are your thoughts on conditions requiring post pyloric placement for tube feeds?
Thank you for clarifying the difference between the Cortrek feeding tube and NG tube.
You’re very welcome!
I was just in the hospital for emergency abdominal surgery. After the surgery was completed I needed the NG tube inserted because my stomach was still distended. My problem with the tube is the insertion process. The nurse had tried it three times. Twice in the right nostril and once in the left nostril and was unsuccessful in all three attempts. And during those attempts, the end of the tube was crunching bone and cartilage while it was being inserted. I was wondering if they make a tube that has the end that’s inserted into the nostril beveled. Almost conical at the end. I think it would cause a lot less heartache and discomfort for the patient if that end was rounded and not just a square cut at the end. Please get back to me and let me know
Hey Michael! Hope you’re doing well with recovery after surgery!
I’m so sorry to hear about your experience regarding NG tube placement. If there’s a list of bedside procedures which are uncomfortable, NG tube placement is easily near the top. So much of it relies on unpredictable anatomy (e.g., enlarged turbinates can narrow the passage) and technique. Most of the tubes (pictured in the post above) have a rounded-off tip to favor pushing structures away rather than cutting through them. I’d be concerned about something more beveled/cone-shaped as the nasal tissue is highly vascularized, and nose bleeds may be even more likely to occur if too much pressure is applied at the tip rather than dispersed over a larger area. 🤷🏽♂️
With all that said, technique and experience are also important. Adequate lubrication is a must (I use lidocaine-based jelly) and positioning is key. Sometimes I’ll even use intravenous sedation to make the patient more comfortable if the benefits of NG tube placement outweigh the risks. Just my two cents!
I love the information you are sharing. I am currently an Nursing Instructor and recently left the bedside. What is very interesting is the gaps in best practice for which tubes to use for nutrition and meds, placement of small bore tubes ie post pyloric or gastric, checking placement of tubes after the initial x-ray verification.
Policy at hospitals is very different than what is taught in school. If you have any suggestions on studies, literature trials that would assist in closing this gap I would love to hear about them. Thanks so much!
This is a nice flow diagram I’ll reference periodically from the American Society for Parenteral and Enteral Nutrition (ASPEN) with the relevant literature and recommendations for the patient population I deal with.
What are the normal parameters for the wall section to be set to for the pt on the Salem sump? Thank you!
I don’t know what is considered “normal”, but for the most part, I have patients on low-intermittent suction in the ICU. I consider “low” to be ~40 mmHg.