Arguably, anesthesiology has one of the largest learning curves right off the bat. Though you’ll rely on the medical knowledge you’ve obtained through medical school and as an intern, clinical anesthesiology is something entirely different. This is what makes entering your first few months a bit unnerving but incredibly exciting! You’re going to subconsciously learn countless tricks and skills to build the foundation you’ll need for the rest of residency. Study hard, work diligently, be a team player and enjoy the ride! 🙂
WATCH ALL INDUCTIONS
In retrospect, one of the greatest things I did as a CA-1 was being present for all inductions of general anesthesia during call shifts. Even if the case wasn’t mine, I would stand and watch the attending, senior resident, and junior resident or SRNA perform the induction/intubation while offering an extra set of hands if needed. Yes, this meant that I never slept on call, but I learned so much just by watching the technique of those more senior than me. Additionally, many of the possible complications of induction (laryngospasm, bronchospasm, anaphylaxis, etc.) occurred in cases I was merely watching. Had I been sleeping, I would have missed out on the opportunity to watch how to quickly diagnose and treat these conditions on a real patient.
EXAMS
As an anesthesia resident, you’ll take a yearly in-training exam (ITE) in each February and an ABA Basic board exam between your CA-1 and CA-2 years. Some programs also administer AKTs (anesthesia knowledge tests) based on how far you are in residency. For example, the AKT-6 is given 6 months into your anesthesia residency whereas the AKT-24 is after 24 months. For fellowship purposes, focus on the ITEs and ABA Basic exam. I’ve written a couple posts about how I prepared for these exams:
- Preparation for the ABA Basic Board Exam
- ITE Preparation
- Best Books and Question Banks for Anesthesiology Residents
- Lessons
Most programs have a didactic lecture series which will provide the basics (pharmacology, physiology, general anesthesia, regional anesthesia, etc.), but it’s up to you to stay motivated and pursue additional enrichment. It’s important to start with the basics and be methodical with your studies. Doing well on these exams will be pivotal for my next point – fellowships.
FELLOWSHIPS
One of the huge differences I found between medical school and residency is how early we have to consider the next (optional) step in our training. I started my fellowship application with over 1.5 years of residency left. Once CA-2 year starts, you should already have an idea who you will be asking for letters of recommendation. Keep in mind, CA-2 year is when most residents will rotate through the various subspecialities (pediatrics, cardiothoracic, ICU, pain, etc.) You will need to ask for advice from more senior colleagues regarding good letter writers and how to best schedule your rotations since things get moving fairly quickly by spring of your CA-2 year.
There’s tremendous variability in the application process among different anesthesiology fellowships, so it’s good to start early and stay on top of everything. Have an updated CV at all times, start drafting a personal statement, and be cognizant of what rotations you schedule during the peak fellowship interview season. Trust me, while it’s difficult to juggle your clinical duties with interviews, you’ll get through it! 🙂
Here are some posts about my fellowship application journey:
- Dual Fellowship Training – Critical Care and Adult Cardiothoracic Anesthesiology
- Fellowship Applications Begin
- Preparing For My First Fellowship Interview
- Dual Fellowship Match Brigham and Women’s Hospital & Harvard Medical School!
- San Francisco Match Dual Fellowship Out-Of-Match Process
STRESS AND INCOMPETENCE
One of the best and worst parts of anesthesiology is the number of ways you can administer an anesthetic. Let’s say you have a thumb fracture repair. Do you want to do a regional anesthetic with a Precedex-based sedation? Or propofol sedation? Or general anesthesia with an LMA? How do you want to induce anesthesia? How will you manage pain post-operatively? Some attendings are very rigid in their practice. Consequently, you’ll learn ten different ways to do the same kind of anesthetic from ten different attendings who think their way is the “right way.” As a trainee, this can be frustrating and very stressful. You’re a product of your teaching, and trying to assimilate different techniques to create your OWN method is what residency is all about! Remain calm and soak up all the knowledge you can. By the time you’re a CA-3, you’ll realize the flexibility inherent to this field and enjoy the fact that you were exposed to so many different styles. 🙂
Now, let’s talk about that feeling of incompetence after you blow virtually every peripheral IV, arterial line, intubation, epidural, or anything in your first days/weeks. It’s demoralizing and humiliating. I remember getting to the hospital literally 30 minutes early just to make sure I had enough time to successfully place the IV on my first patient of the day. It literally was a “make or break” ordeal which dictated how I felt about myself the rest of the morning. 🙁
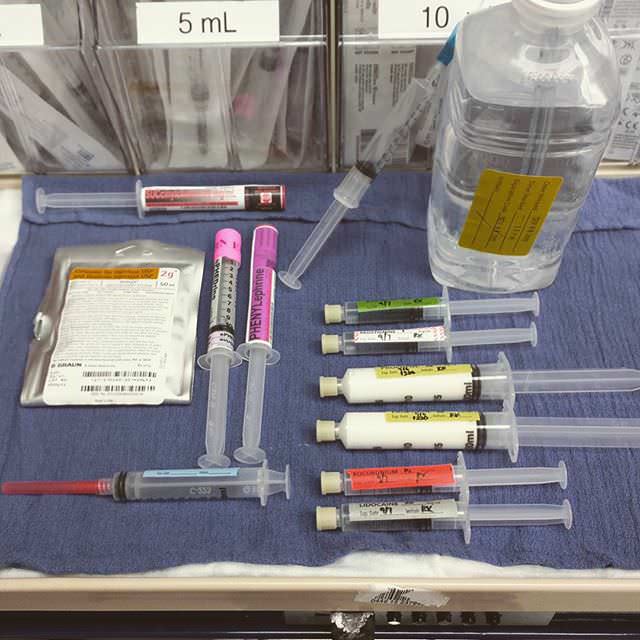
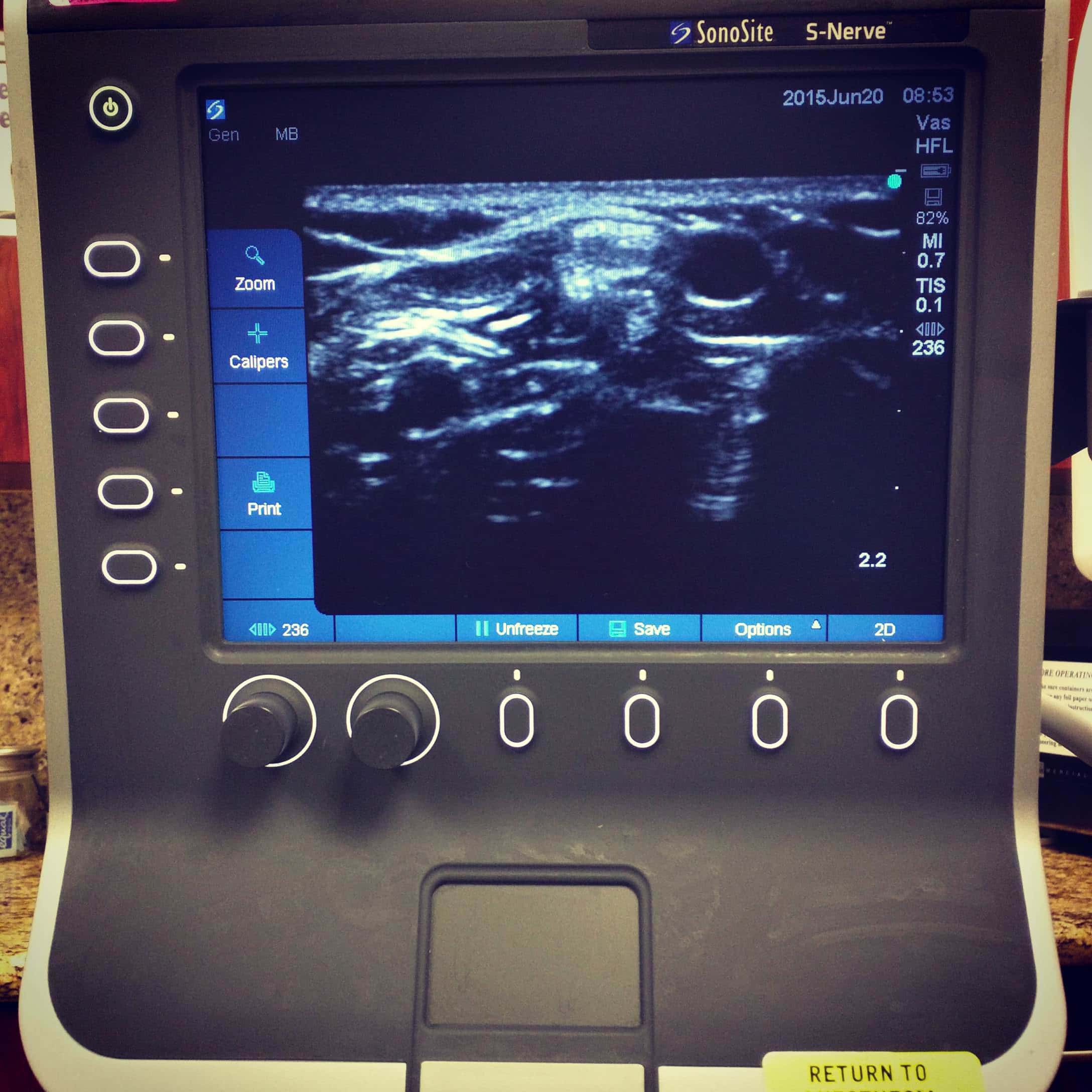
I promise the more you do, the better you’ll get. Eventually you’ll be missing intubations because the airway is indeed “difficult” and worthy of more advanced equipment. You’ll need to get that ultrasound for line placement because not even the most experienced attendings can cannulate a peripheral vein. As your skills grow, you’ll also be more comfortable missing an easy airway or IV from time to time. A hallmark of anesthesiologists is our ability to remain calm in stressful situations and not be bothered by the simple things. In moments where you feel like you “suck at everything”, take a deep breath and realize that we have all gone through this. It’s a part of the journey, and tomorrow is a new day to practice more.
FRIENDSHIPS AND LOGISTICS
Build relationships with people who you will be working with on a daily basis – nurses, techs, pharmacists, housekeeping, surgeons, administration, etc. You’ll need to master the workflow as much as the actual skills inherent to perioperative care. How do you turn a room over quickly? How do you streamline your clinical duties while simultaneously helping others do the same? As you get farther in residency, your colleagues will seek your opinions regarding optimization for complex cases, pain management, and even the occasional line placement. Be there for them, and they will return the favor. After all, medicine relies on good communication and the collective efforts of all.
So in conclusion, residency is difficult. The hours are long and unpredictable. You’ll spend many call shifts wondering why you ever became a physician. It’s in those moments that you must remember what got you here. You made it through college and completed medical school. You’re a doctor. You have an extraordinary knowledge base and therefore an implicit responsibility to build on your training thus far to improve the wellness of others. Let that alone be a motivating factor. 🙂
I’ll update this post periodically, but drop me a comment if you have any specific questions!







I m a doctor from India, Starting my residency in Anaesthesia in a reputed institute in India, How should i prepare myself if i want to work or study in Harvard or other big medical schools.. Kindly guide.
It doesn’t matter where you want to work, you’ll still need to go through the process of getting certified to work in America (for example, taking all the USMLE Steps). I’m honestly not sure about the rest of the details regarding the process since I didn’t train abroad.