Reading a chest x-ray (CXR) is an incredibly important aspect of acute care medicine and a skill that all healthcare providers should at least have some comfort in doing. The key for interpreting any radiographic image is having a methodical approach you follow every single time, no matter how simple or complex the initial impression is.
Before I even start interpreting the CXR, I have to know I can trust my findings. Here are the things I assess:
- Identify the film. Make sure the patient name and medical record number match the patient in question.
- Is this an anterior-posterior (AP) or posterior-anterior (PA) film? The latter is ideal as x-ray beams traverse the patient from back to front and minimize artificial enlargement of mediastinal structures. AP films are the traditional “portable” films we take in the ICU, but since the heart is positioned farther from the film compared to a PA, it appears larger than it really is. Consequently, AP images tend to show cardiac magnification and mediastinal widening.
- Does the CXR include all the anatomy you need? Sometimes the image is zoomed in and excludes the lateral edges of the ribs and/or costrophrenic angles.
- Is the CXR appropriately penetrated? Under-penetrated films (appear white) tend to falsely accentuate pulmonary markings and obscure diaphragmatic borders. Over-penetrated films (appear black) make it difficult to really assess anything. I try to look for the silhouette of the thoracic vertebrae or disc spaces through the heart to determine appropriate penetrance.
- Is there a rotational component to the CXR? The thoracic vertebrae should form a vertical column and each vertebrae should maintain an equidistant relationship with the medial aspect of each rib in most cases. Rotation can falsely suggest pathologies like tracheal deviation, cardiomegaly, and pulmonary artery enlargement.
- The posterior aspect of each rib is what we’re usually looking at on the CXR. They’re more visible and run horizontally. The anterior aspect of each rib is harder to see, but they slant downward at a 45 degree angle. Visualizing 9-ish posterior ribs indicates adequate inspiratory effort.
In general, we’re working in non-ideal conditions in the ICU. We have to accept the imaging we get but carefully interpret our radiographic impressions in the context of potential confounders regarding the quality of the CXR and the technique by which it was obtained.
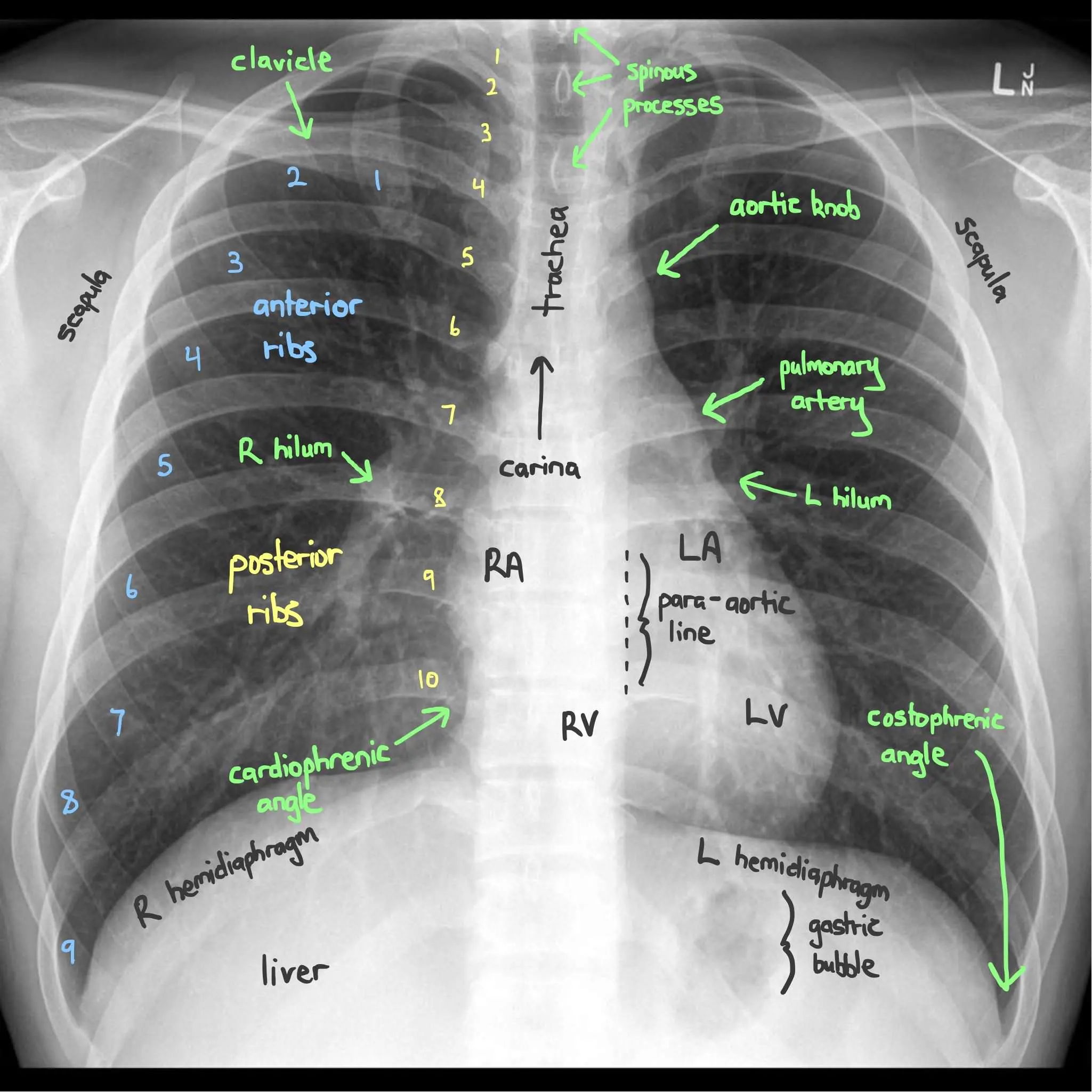
I use the popular A-B-C-D-E method of structuring my interpretation. It stands for pretty much the same thing as the A-B-C-D-E in trauma surveys. 😀
- A – Airway (tracheobronchial tree evaluation)
- Is the trachea midline? Does it contain any defects or strictures?
- Find the carina and takeoff of the right and left mainstem bronchi
- B – Breathing (lung and pleura)
- Assess the lung fields, fissures, costophrenic angles
- Atelectasis, pleural effusion, parenchymal consolidation, mass, pulmonary edema?
- C – Circulation (cardiac, aortic arch, pulmonary vessels)
- Full clarity of the heart borders?
- Cardiac position and size, widened mediastinum, aortic arch, pericardium issues, hilar fullness, cephalization of pulmonary vasculature?
- D – Disability (bony pathology from outside to in)
- Examine all bony structures ranging from the humerus and vertebrae to individual ribs anteriorly and posteriorly – any fractures or abnormalities?
- E – Everything Else
- Foreign objects
- Tubes, lines, and drains: endotracheal tube, central line, PICC, PA catheter, chest tubes, etc
- Devices: AICD, pacemaker
- GI tract – gastric bubble, free subdiaphragmatic air
Drop me a comment below if you have any questions or recommendations regarding CXR interpretation! 🙂






Thanks so much it’s so helpful
This is so so helpful doc, how about making a video of the normal? I just trust you can make good one. Thank you very much
While I am not in an ICU setting, I have been interested in your posts. Thank you for taking the time out to create these educational and informative resources.
You are very welcome, Maria! Thanks so much for the comment! 🙂
Nice job SIR !
Thank you!
Thank you! I was looking for this to be written in a simplified and summarized way.
Glad you found the post helpful!
Really helpful. Keep up the good work.
Thank you! 🙂
NP student here and I follow your pg on IG. I was looking for chest x-ray reading techniques when I ran into your page here. Love it! Keep up the good work!
Thanks so much for the comment! You are very welcome!
Sir,
Could you please make an article perhaps in the future regarding all the possible findings in an xray in various pathologies of the lungs and the heart.
Thanks for the comment! Unfortunately that’s a very complex task, and I just don’t have the time. I like sticking to the basics. 🙂
This blog is very informational. I love it
Thanks Matteo! 🙂