CentriMag devices are implanted for acute right and/or left-sided circulatory support but often times used for extended periods of time for patients with acute heart failure awaiting a heart transplant. With CentriMag devices, patients can ambulate and stay conditioned in preparation for their orthotopic heart transplant. These devices rely on MagLev technology whereby a free-floating rotor suspended within a constantly adjusted magnetic field delivers blood flow in an environment with minimal shear forces and stasis to reduce cell trauma and clots, respectively.
My anesthetic plan for CentriMag placement includes: general endotracheal anesthesia, arterial line, central venous catheter (often times with PA catheter) and intraoperative transesophageal echocardiography (TEE). So how are these devices placed for right and left ventricular support?
After a median sternotomy and systemic heparinization, a graft is sewn onto the ascending aorta with an aortic cannula placed within the graft prior to venous cannulation of the right atrium. Cardiopulmonary bypass (CPB) is initiated. The LVAD CentriMag drains blood from the left ventricular (LV) apex and returns it to the aortic graft. The RVAD CentriMag drains blood from the right atrium via a large venous cannula and returns it into the pulmonary artery (PA) via the right ventricle (RV). CPB is weaned, protamine is administered to reverse systemic heparinization, hemostasis is achieved, and the incision is closed in anatomic layers with sutures and stainless steel wires for the sternum.
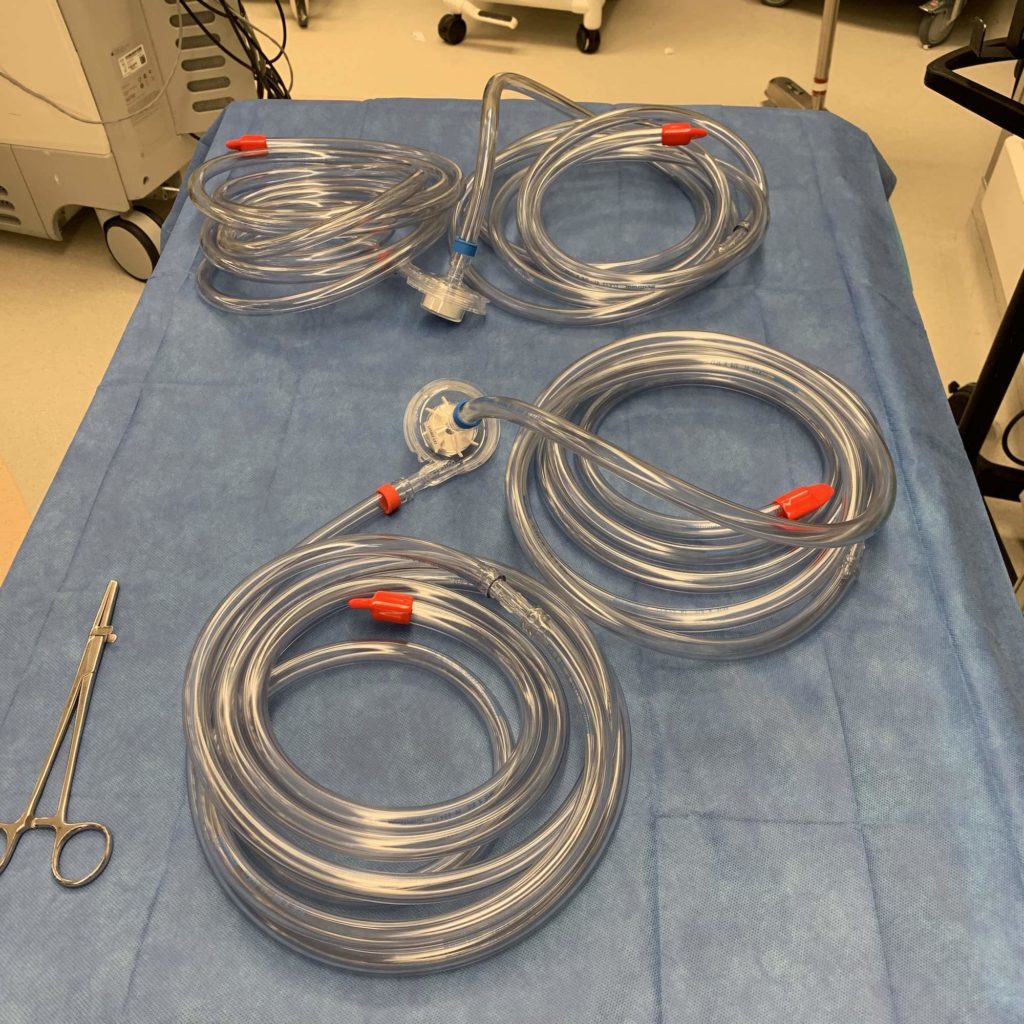
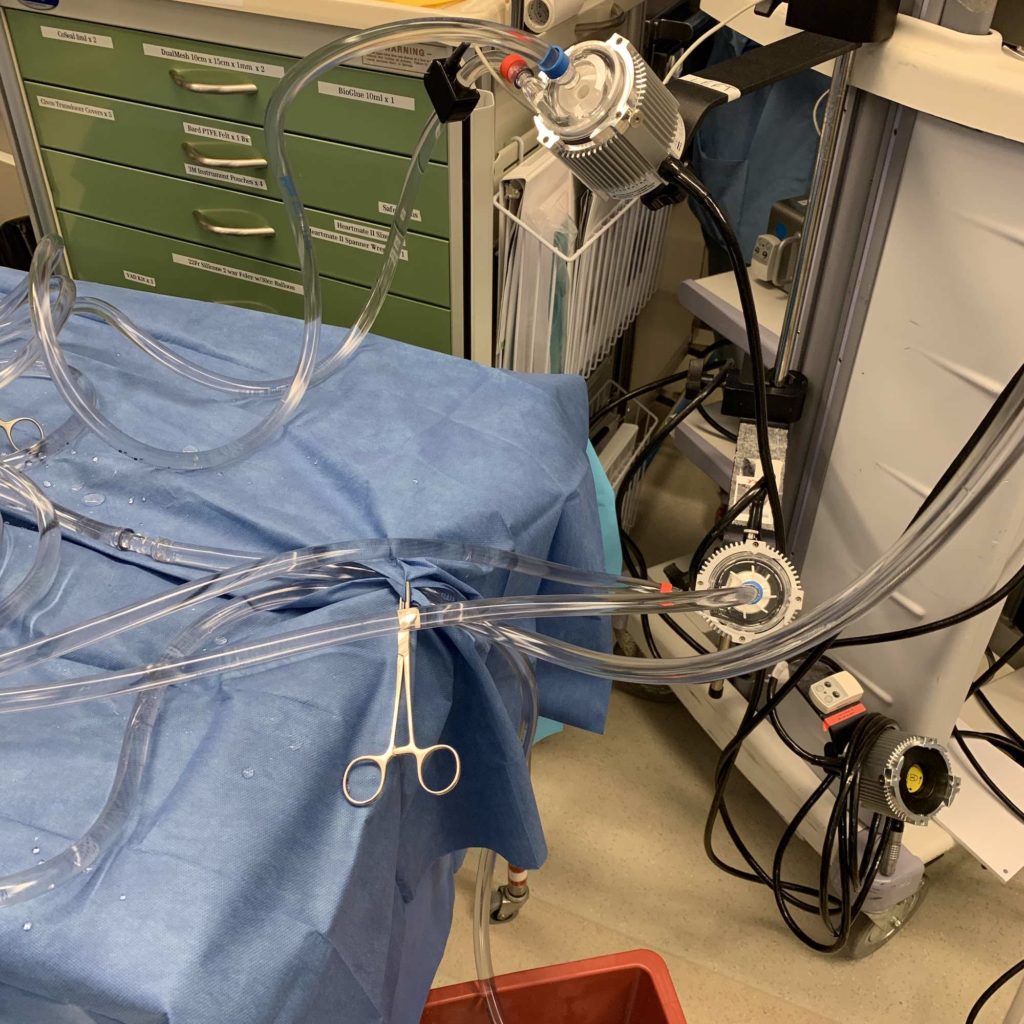


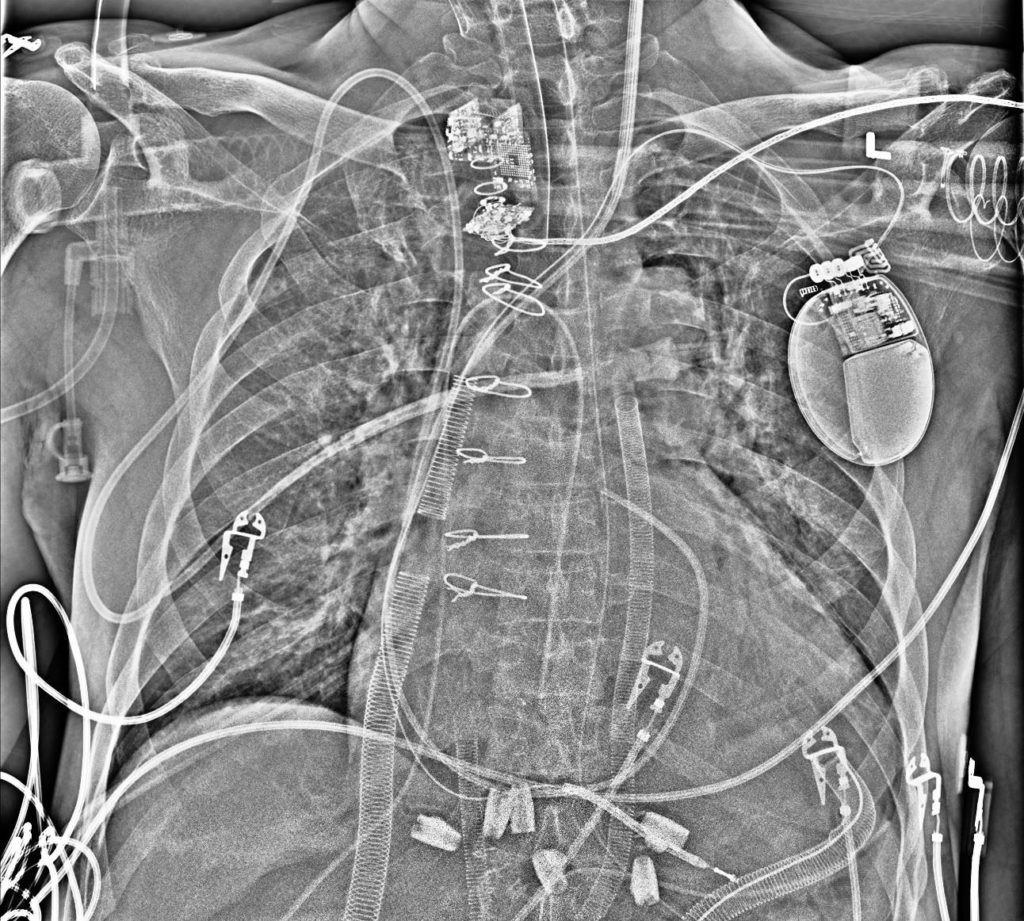
In the post-operative x-ray above, you can see the CentriMag BiVAD cannulas with other things to note: right internal jugular introducer with PA catheter, pacemaker/ICD leads, endotracheal tube, orogastric tube, sternotomy wires, two mediastinal chest tubes, one left pleural chest tube, one right pleural chest tube.
Drop me a comment below with questions! 🙂






I am a survivor of having a centrimag and also a bivad until my heart transplant. Thank you for all you do!
That’s incredible, Rachel! Thanks for sharing, and I hope you’re doing well! 🙂