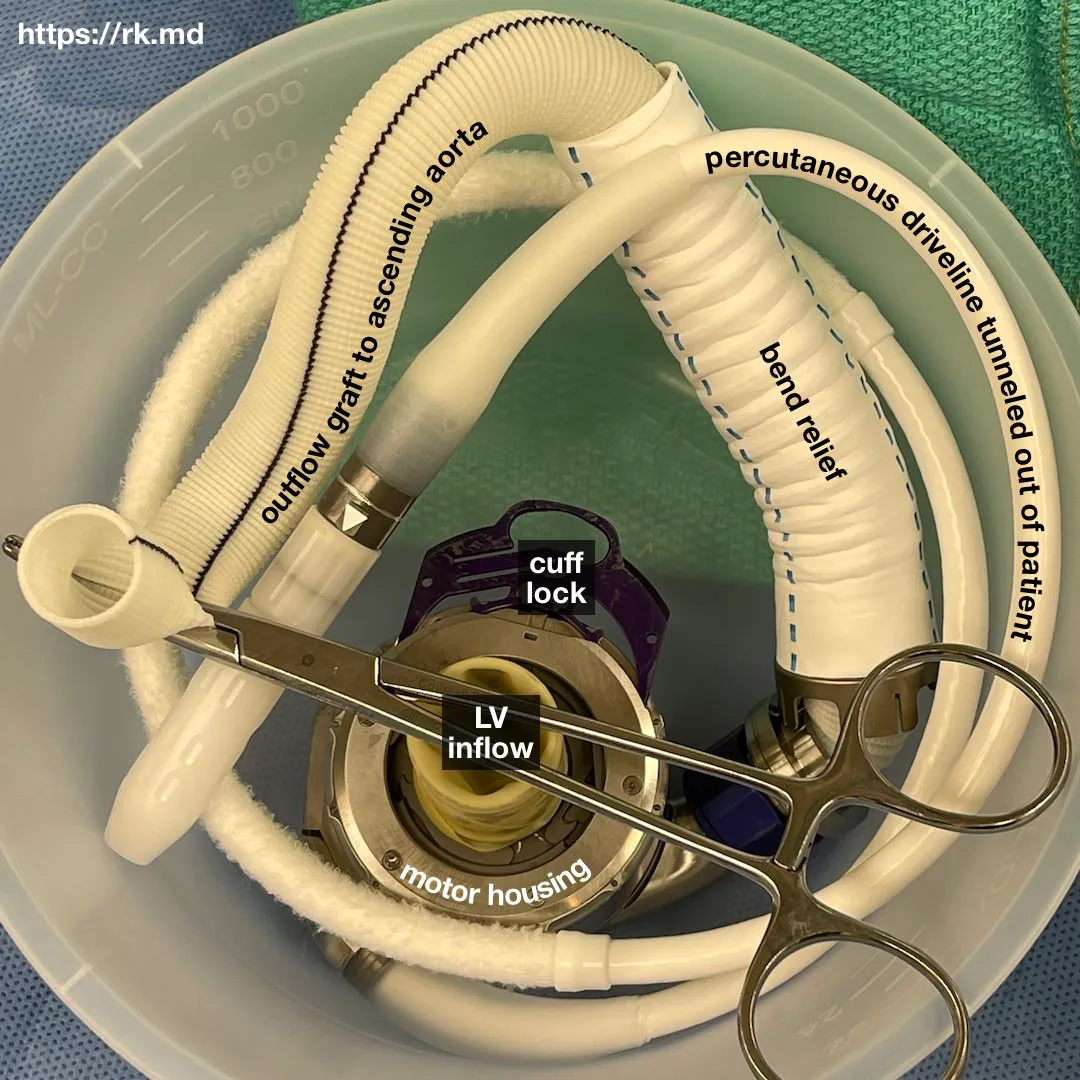
Left ventricular assist devices (LVADs) like the HeartMate 3 are routinely being implanted as a mechanical circulatory bridge-to-transplant (BTT) or destination therapy (DT). My anesthetic plan for LVAD placement includes general endotracheal anesthesia, arterial line, central venous catheter (oftentimes with PA catheter), and intraoperative transesophageal echocardiography (TEE). In particular with TEE, I’m looking for aortic insufficiency, clots, and intracardiac shunts like ASDs/PFOs (this is where a bubble study comes in handy!)
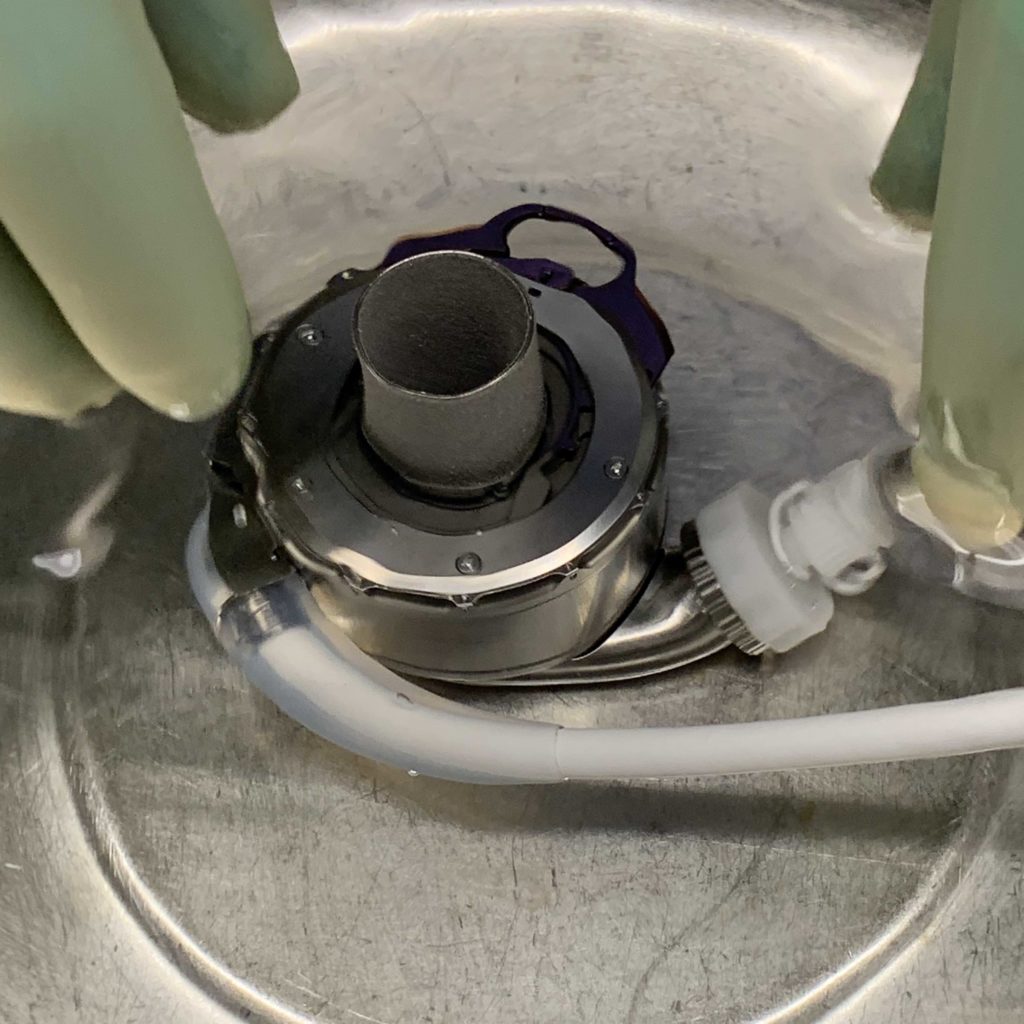
The operation starts off with a median sternotomy followed by arterial cannulation (ascending aorta) and venous cannulation (bicaval). After initiating cardiopulmonary bypass (CPB), the LVAD’s inflow cannula is sewn onto the left ventricle (LV) and the outflow cannula is sewn onto the ascending aorta in an end-to-side fashion. An outflow graft clip is placed with subsequent de-airing of the LVAD system. CPB is weaned, protamine is administered to reverse systemic heparinization, hemostasis is achieved, and the incision is closed in anatomic layers with sutures and stainless steel wires for the sternum.
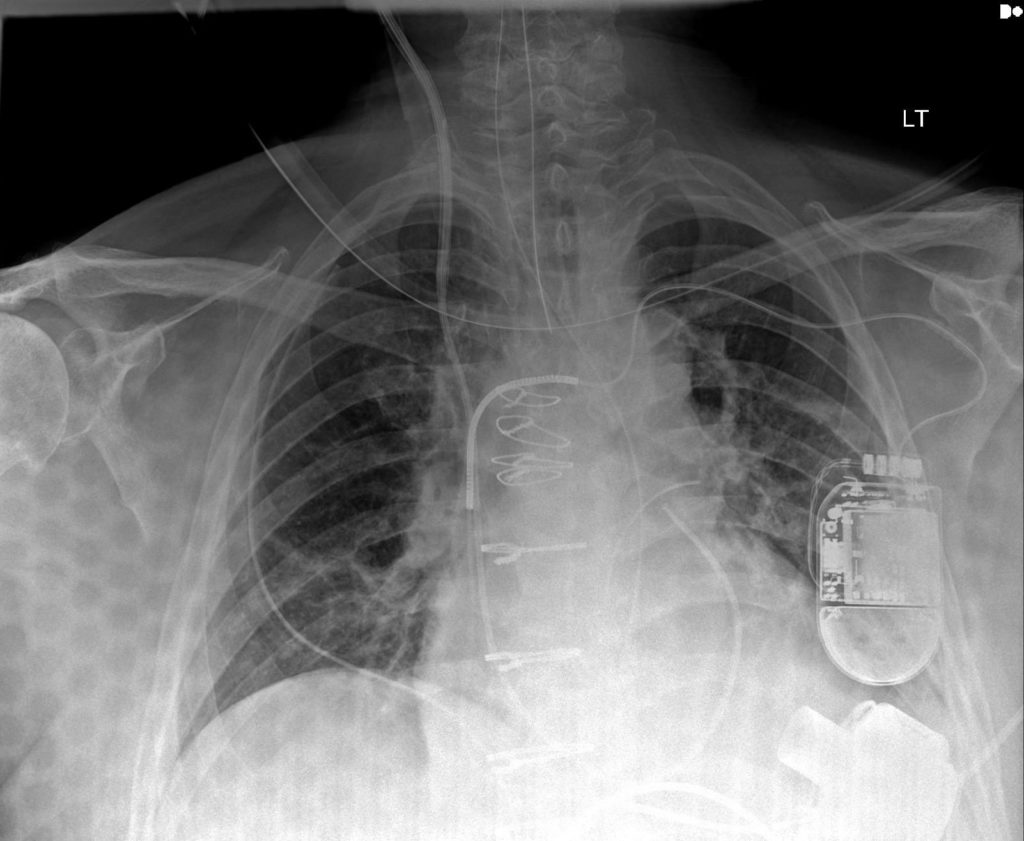
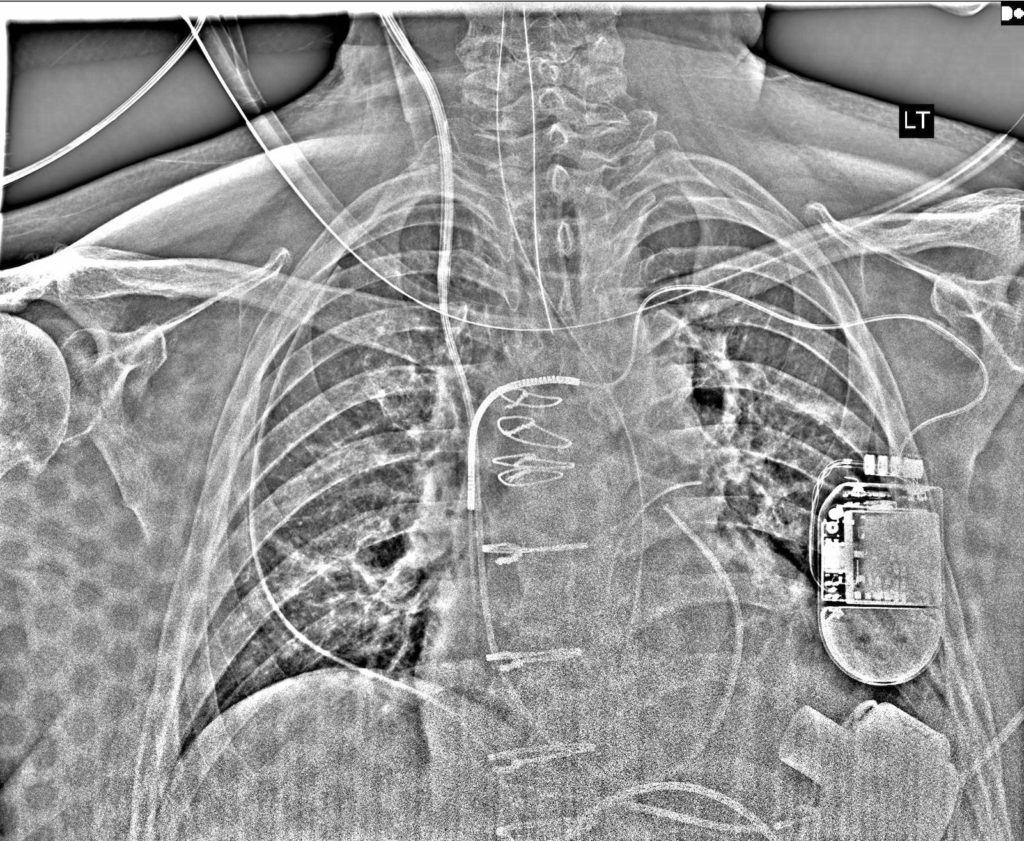
In the x-rays above, you can see the HeartMate 3 LVAD inflow adhered to the left ventricular apex. Other things to note on the x-ray: right internal jugular introducer with PA catheter, pacemaker/ICD leads, endotracheal tube, orogastric tube, sternotomy wires, two mediastinal chest tubes, one left pleural chest tube, one right pleural chest tube.
Drop me a comment below with questions! 🙂