Tracheoinnominate fistulas (TIFs) are rare (0.1 – 1% incidence) but potentially life-threatening complications of tracheostomy. A TIF occurs when communication forms between the trachea and the innominate (“brachiocephalic”) artery leading to potentially fatal bleeding and airway compromise. Patients at higher risk for TIFs include those who require prolonged mechanical ventilation, have a history of radiation therapy to the neck, or have had multiple previous tracheostomies.
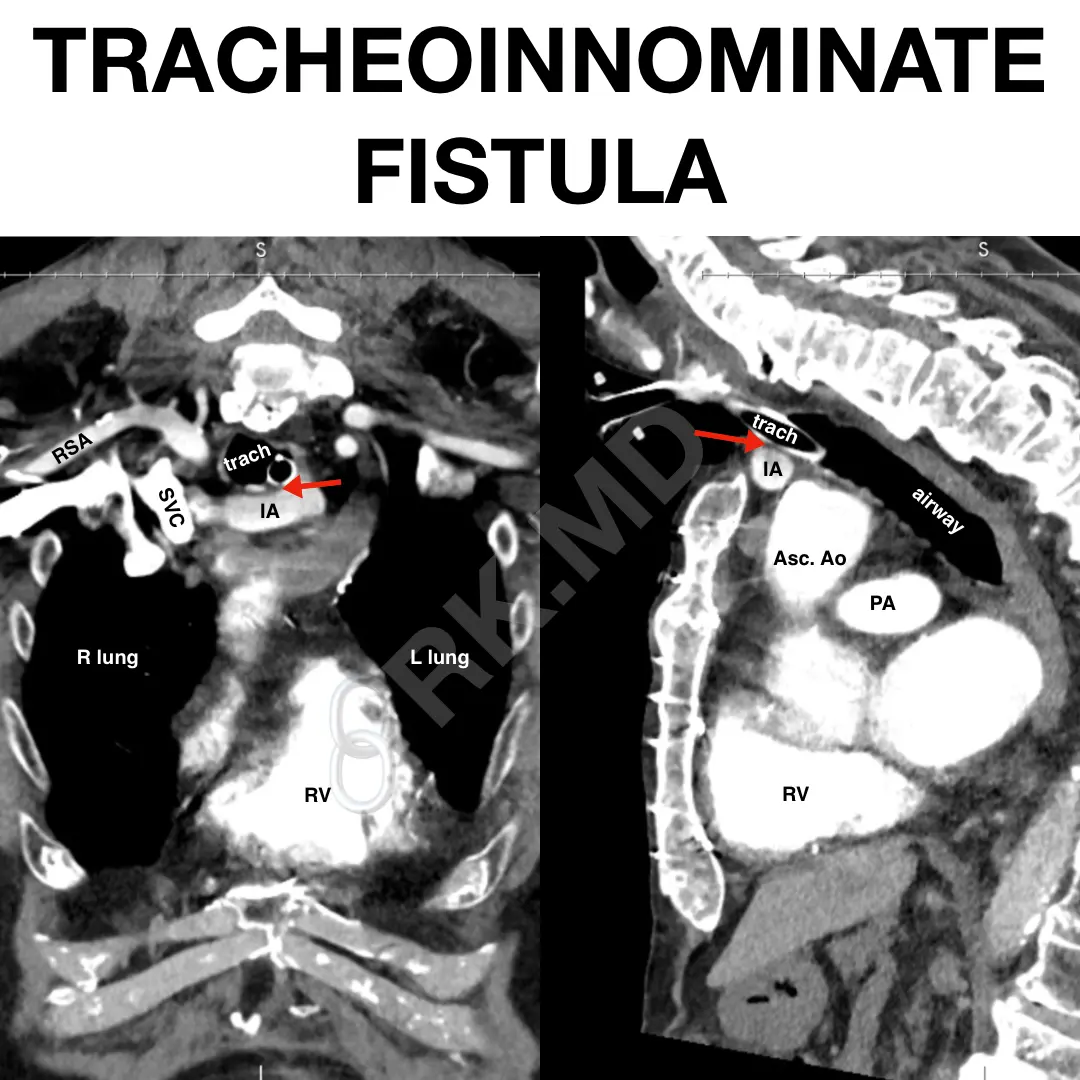
In the pictured coronal (left) and sagittal (right) chest CT images, the red arrows show the trach tube traversing near the innominate artery (IA) without a separating tissue plane identified. This – is – scary!
The symptoms of a TIF can be subtle at first (e.g., coughing, dyspnea, small sentinel bleed) but can progress to massive airway bleeding and obstruction. Therefore, early diagnosis is critical and is largely centered on clinical suspicion coupled with confirmatory imaging.
The treatment of a TIF involves emergent airway management and surgical intervention to address the fistula, including ligation of the innominate artery, resection/repair of the trachea, or insertion of a covered stent to seal the fistula.